July 29, 2024
Millions of people all over the world deal with some form or another of chronic illness every single day. One of the most widespread of these chronic conditions involves the injury or disease of one or more of the tendons in the body, commonly known as tendinopathy. Since tendons are the body members that attach muscle to bone and make movements possible, once a given tendon becomes injured in some way it can take a long time for it to regain the health that it once had.
This is because if the tendon in question is located in a major joint area, it can be very difficult to effectively immobilize it and allow the healing process to begin. In cases such as these, rest may not be enough to heal the tendon and more proactive medical measures may need to be taken to allow individuals suffering from chronic tendinopathy to regain full function.
This article will take a closer look at one of the more promising tendinopathy therapies in use today, known as ultrasound-guided dry needling. It will discuss what the treatment involves, how it is performed, and what some of the advantages of this course of action provides.
Before tendinopathy is discussed it will be useful for readers to have a little information about tendons. Tendons gain much of their overall strength and durability from the closely packed fibrous collagen structures that mostly make them up. In the case of a tendinopathy, the collagen fibers become torn, disorganized, and remain chronically unrepaired.
Once the endotendon and the paratendon become injured and stay that way for a minimum of three months, a diagnosis of chronic tendinopathy is usually given. It is important to note that whole or even partial ruptures of the tendon are not necessarily considered to be tendinopathies because they may not end up being chronic conditions.
Tendinopathies tend to be overuse or misuse injuries, and because of this they disproportionately affect athletes, especially ones that may only play their sport on weekends. Once an individual develops this condition, it can have drastic effects on their athletic performances. This, in turn, can have a dire effect on the careers and therefore the earnings of high-level and elite athletes.
Tendinopathies have been around as long as people have, and because of this, there have been many attempts at therapies to resolve this age old issue. In many modern cases, eccentric and concentric stretching exercises are prescribed by physical therapists, along with courses of either applied deep heat or cold. Certain medications are also commonly used to try to manage pain and inflammation, and in some cases, patients elect to attempt a surgical intervention. That said, many people have found relief by the use of treatments such as acupuncture, and a modern version of this is the therapy known as ultrasound guided needling.
Using needles in one way or another to treat chronic tendon injuries has been an accepted therapy for some time in the form of acupuncture. While acupuncture is still widely used as an intervention, many contemporary physicians now use slightly larger needles in various ways to try to stimulate healing within affected tendon tissues. Some of these modern therapies involved injecting tendons with one substance or another, which in many cases involve corticosteroids.
An even more cutting edge therapy is known as needling, and during this procedure, small needles are themselves used as the treatment. The procedure to do so is fairly easy to understand. First, most patients are provided with a topical anesthetic in order to numb the skin in the area of the body where the needling will take place. After this, a small amount of anesthetic is applied to the tendon that will be the target of the treatment, making it impervious to pain. After this part is accomplished, small 22 gauge needles are used to penetrate the affected tendon, allowing nutrient rich blood to flow into the region that is suffering from a damage to the collagen fibers.
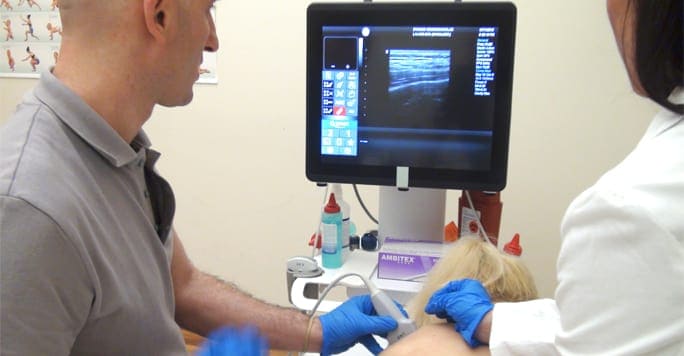
Ultrasound comes into the picture as a way for the physicians to guide the needles to the areas where they will do the best. Ultrasound is applied to the affected tendon, and this produces a feedback that the ultrasound technicians can decipher and analyze. Healthy tendon tissue provides once kind of signal, while unhealthy or damaged tissue provides another. By zeroing in on the damaged tissue using pulses of sound, doctors and physical therapists can deliver medical care to affected tendons with more accuracy than ever before.
This novel approach to the treatment of chronic tendinopathy has shown much promise in some studies and clinical trials testing the therapy. According to researchers that took part in a 2009 study at the Department of Orthopedic Surgery at the University of Michigan, 80% of the patients that took part in the treatment regimen enjoyed an average 90% improvement in their symptoms as well as a complete recovery in several cases. This study also indicated that needling as a method to treat chronic tendon pathology can be effective even if patients do not receive injections of corticosteroids in conjunction with the needling treatment.
Compared to the treatment period that is required for various other chronic tendinopathy therapies, the treatment period observed for dry needling is fairly short. In many instances, patients will receive anywhere from two to six treatments with an interval of a couple of weeks between visits to the doctor’s office. After the final procedure has been performed, most individuals will be asked to make follow-up visits to their physician at 4 weeks out and again at 12 weeks.
When it comes to helping patients overcome the difficulties of chronic tendon disease with needling, the advantages of using ultrasound become very clear to see. For one thing, in the past, many physicians were forced to rely on the patient for information about exactly where the problem was originating from. Given the fact that many patients were provided with pain medication before palpation, this resulted is less accuracy in terms of diagnosing specifically where the treatment should be delivered.
By using ultrasound, not only can doctors and physical therapists precisely find the problem spot, they can also guide the needles directly to where they are needed the most. This minimizes false positives, saves the patient time and discomfort, and makes these kinds of procedures safer and more effective than ever before.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: