January 2, 2025
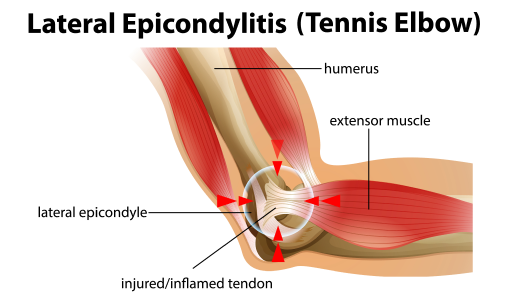
 Chronic lateral epicondylitis — aka tennis elbow – is a painful condition caused by repetitive overuse of the forearm wrist extensor muscles that attach to the epicondyle of the humerus bone, just above your elbow. Although tennis elbow can occur at any age, the condition is most commonly reported in adults aged 35-60. Despite its nickname, only about 20 percent of tennis players actually experience tennis elbow.
Chronic lateral epicondylitis — aka tennis elbow – is a painful condition caused by repetitive overuse of the forearm wrist extensor muscles that attach to the epicondyle of the humerus bone, just above your elbow. Although tennis elbow can occur at any age, the condition is most commonly reported in adults aged 35-60. Despite its nickname, only about 20 percent of tennis players actually experience tennis elbow.
Learn about the causes and symptoms of chronic lateral epicondylitis, other conditions that mimic its symptoms, and why high resolution ultrasonography is far superior to MRI for diagnosing and treating elbow injuries.
In medical jargon, the suffix “itis” indicates an inflammatory condition, but in the case of lateral epicondylitis — as well as other tendon pathologies – this is usually a misnomer. In general, tendon tissue is avascular, meaning it has a limited blood supply, and microscopic evaluation of tendon tissue rarely shows signs of inflammation. In most cases, tendon injuries are marked by the degeneration of fibroblasts and disarray of collagen fibers.
While standard treatments for inflammation – such as ice, compression and NSAIDs – may help to soothe tennis elbow symptoms in the short run by desensitizing nerves, long-term relief requires a multifaceted approach aimed at realigning collagen fibers and rehabilitating the affected structures.
Early symptoms of tennis elbow begin as pain over the lateral elbow that intensifies during activity and abates during rest. Pain usually arises within 24-72 hours after repetitive wrist extension, with maximum tenderness upon palpation of the extensor carpi radialis brevis (ECRB), which is often the afflicted tendon. Even with reduced activity, tennis elbow symptoms can persist for months, with some cases taking over a year to resolve.

The intensity of tennis elbow symptoms often correlates with the severity of injury.
In conventional medicine, imaging is rarely used for diagnosis of tennis elbow. Instead, doctors rely on reported symptoms and results from the clinical exam. Only when treatments fail to alleviate persistent symptoms is MRI considered, to look for other causes such as osteophytes, degenerative joint disease, osteochondritis dissecans, or stress fractures, all of which share the same symptoms. However, in many cases, the limitations of MRI make it an impractical and ineffective diagnostic tool.
MRI’s shortcomings include:
By comparison, ultrasonography provides a clinically-friendly diagnostic tool, with more extensive capabilities than MRI.

In addition, high resolution dynamic ultrasonography can distinguish tendinopathy from tendon ruptures. In most cases, patients with tendon tears also have partial ligament tears and/or ligament laxity, conditions that are difficult to visualize with MRI.
According to recent research, a unique imaging technique called stress ultrasonography can directly visualize the ulnar collateral ligament (UCL) – an elbow ligament that is frequently injured during repetitive overhead movements. Stress ultrasonography allows for assessment of ligament laxity, a distinct advantage over MRI.
A significant disadvantage of symptoms-based diagnosis is that other less common contributing factors may be overlooked. In fact, research indicates that, due to inappropriate handling of the condition, a substantial number of patients diagnosed with lateral epicondylitis do not experience positive therapeutic outcomes.
Lateral epicondylitis is only one of many conditions that affect the lateral elbow region and exhibit the same symptoms as tennis elbow. Failure to consider alternative causes of tennis elbow symptoms can prolong the patient’s suffering and potentially worsen the condition.
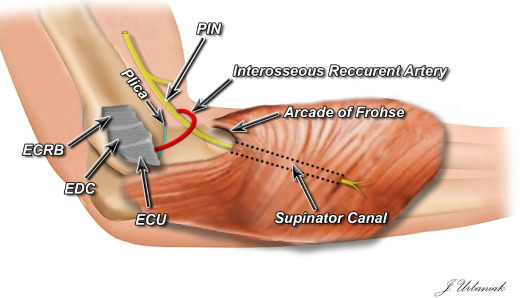
Diagnostic ultrasound enables the clinician to thoroughly examine the elbow and its surrounding tissues and structures. With dynamic ultrasound, doctors can assess how the various structures interact while in motion, compare the injured and uninjured elbows, and test for tissue laxity using sonoelastography.
If you’ve ever had an MRI scan, you know what a costly and uncomfortable ordeal it can be. In many cases, doctors are unable to detect tissue damage based on MRI, making the procedure a total waste of time and money.
The clinic at NYDNRehab features the highest resolution ultrasound equipment currently available, with capabilities for sonoelastography and microvascular imaging. Our clinical director, Dr. Lev Kalika, is a recognized expert in diagnostic ultrasonography, credited with multiple scientific publications on the procedure.
If you suffer from chronic lateral epicondylitis or other chronic pain syndromes, we conduct same-day diagnostic ultrasound imaging in the comfort of our Midtown Manhattan clinic, for a fraction of the cost of MRI.
Contact NYDNRehab today to get a quick and accurate diagnosis, and a personalized treatment plan that gets fast results.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: