Running is a great form of exercise, with numerous advantages for physical and mental health. For many, running provides an inexpensive and easily accessible way to manage weight, boost cardiovascular fitness and neutralize stress. But running subjects the body to powerful ground reaction forces that can potentially cause injury.
The high-tech runner’s lab at NYDNRehab uses a data-driven approach to analyze running gait in 3 dimensions, to identify mechanical deficits that can increase your risk of injury. Our state-of-the-art clinic features advanced technologies for accurate and effective gait retraining, to help you prevent injuries and improve performance. Our regenerative therapies speed up post-injury recovery, to get you back on the road ASAP.or
3D gait analysis using advanced technologies can give us valuable insights into biomechanical deficits in running gait, but gait analysis alone cannot give us a clear picture of running injuries. Running gait analysis only gives us data about joint angles, force loads, stride, foot pressure, muscle firing patterns, and other mechanical parameters.
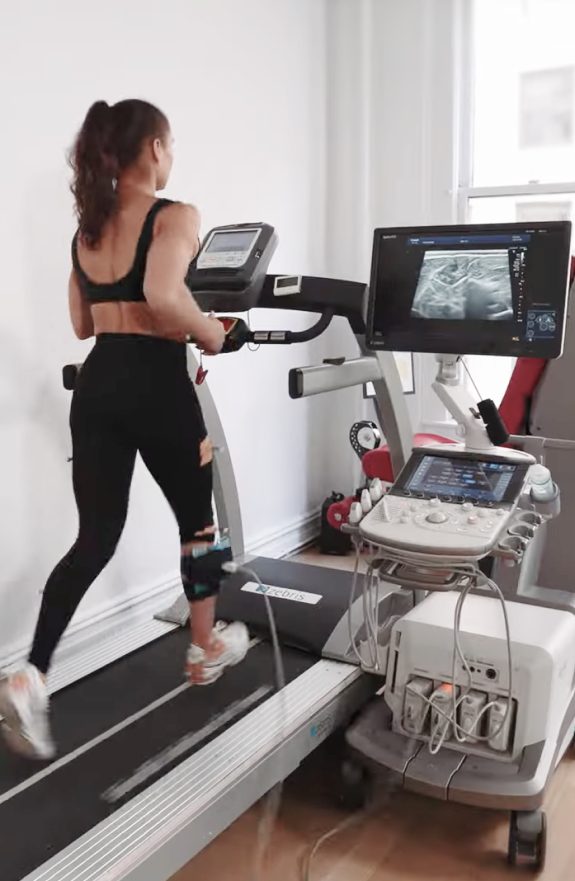
To understand the type and extent of injured tissues, we use high resolution diagnostic ultrasonography in conjunction with gait analysis data. Dynamic real-time ultrasound lets us visualize damaged tissues in motion, to see how they impact and interact with other tissues and structures.
Accurate interpretation of ultrasound images requires extensive experience in clinical examination and an in-depth understanding of running pathologies. With over 20 years of experience in sports medicine, coupled with extensive training and research in musculoskeletal ultrasonography, Dr. Kalika has established himself as a leader in running gait analysis and injury treatment in NYC.
We conduct our gait analysis and ultrasound exam on-site at our clinic. Our cutting-edge technologies and regenerative therapies are designed to accelerate injury healing and correct mechanical gait deficits so you can get back on the road with confidence.
Dr. Kalika has dedicated his life’s work to finding innovative and effective ways to treat and prevent injuries, movement disorders, and pain syndromes. With over 15 years of experience performing diagnostic ultrasonography in conjunction with 3D gait analysis, Dr. Kalika has gained extensive insight into common mechanical causes of running injuries. He has used his knowledge to develop one of the most advanced 3D running labs available in a private clinical setting.
NYDNRehab clinical director Dr. Lev Kalika is an internationally recognized expert in diagnostic ultrasound imaging, with multiple research papers to his credit. Dr. Kalika has studied with some of the world’s most prestigious experts in diagnostic ultrasonography, and has attended multiple international conferences on the topic.
Ultrasound imaging has multiple advantages over other imaging tools like MRI, Xray and CT scan. The musculoskeletal ultrasound equipment at NYDNRehab has the highest resolution available in NYC, for clarity in diagnosing injuries to muscles, tendons, nerves, bones and joints.
In 70% of cases, diagnostic ultrasonography gives us insight into whether structural damage is the cause of pain and dysfunction, or if it reflects compensation patterns developed due to other issues. To make our interpretation of running gait analysis data fully diagnostic, ultrasound helps us visualize both recent structural damage and older injuries that may no longer cause pain, but still contribute to inefficient movement patterns. Only by visualizing both old and new injuries can we create a truly effective treatment plan.
Dr. Kalika is an active member of the American Institute of Ultrasound in Medicine (AIUM), and is currently developing his own unique approach to Dynamic Functional Ultrasonography.
Three-dimensional kinematics measures joint angles at every phase of the running gait cycle, including angles in the transverse (rotational) plane where most running injuries occur.
Our Zebris instrumented treadmill is embedded with pressure sensors and specialized software to record kinetic forces and trace the foot's center of pressure (CoP) throughout the gait cycle. Any gait analysis is incomplete without this information.
Our state-of-the-art ultrasound equipment lets us dynamically visualize your muscles and joints during running in both gray-scale and M-mode. Our customized probe holder gives us real-time images of your body's structures in motion. When matched with kinematic data, we get a clear picture of myofascial and intermuscular coordination, and we can estimate eccentric, concentric and isometric muscle actions.
Once we collect and analyze your data, you receive a 17-page report detailing your personalized 3D gait analysis, complete with training recommendations for improving your running performance. Your report includes personalized data on 3D kinematics, foot pressure analysis results, assessment of spatio-temporal running parameters – e.g. overstriding, vertical oscillation, strike patterns, cadence and stiffness.
NYDNRehab’s team of sports physical therapists and chiropractors have advanced training in running gait analysis and biomechanics. Our user-friendly STT software leverages AI to analyze collected data and categorize your running profile (overstriding, knee overdrive, etc.). Data from our foot pressure analysis gives us a window into the forces mediated by the inner foot during running.
UNOSO dynamic motion ultrasonography combined with our top-of-the-line high resolution Apollo ultrasound equipment let us visualize muscle action in real time as you run. No other gait analysis technology can visualize core muscle activation during running. We can position the UNOSO probe over a painful area such as the knee meniscus or shin to detect inefficient load transfer and loss of control. We can also detect injury or strain in a particular muscle, ligament or tendon, and identify fascial tears and densifications.
The Runner’s Clinic at NYDNRehab features research-grade technologies for measuring and quantifying running performance data. Our advanced motion ultrasonography capabilities let us view the body’s structures in real time, while the patient is running.
Real-time ultrasound imaging paired with objective data gives us an accurate baseline overview of running gait mechanics, allowing us to customize an effective and measurable protocol for personalized gait retraining. The specific configuration of our 3D running lab is based on the latest evidence-based motion analysis research.
Conventional 2D gait analysis is generally subjective, based on observations of running gait via amateur video. Even if you add objective factors like joint angles, and spatiotemporal parameters like speed, stride length, and phases of the gait cycle, you only get a superficial overview of the subject’s gait mechanics. And unless you have a treadmill with the capacity to measure force and pressure, you cannot accurately assess foot mechanics.
While conventional analysis may be useful for suggesting basic improvements in running gait, it does not reveal critical mechanical deficits that can undermine performance and lead to injury. In many cases, runners are given generic explanations for their pain, such as weak glutes, tight hip flexors, weak or tight calves, etc. However, exercises prescribed to target those muscles often fail to eliminate pain or render satisfactory improvements in running gait.
In 95% of runners who do not experience pain while running, simply looking at gait mechanics, even with the most sophisticated equipment, is not enough to get a full and accurate picture. It is only when we visualize how the body’s structures interact during running that we get a clear idea of how to make improvements. The running lab at NYDNRehab features diagnostic motion ultrasonography, a new technology that allows us to look at muscle and joint action in real time. With motion ultrasonography, we are able to sync 3D data with high-resolution imaging, to detect issues with muscles, tendons, fascia, ligaments and joints.
This unique combination of technologies helps us to confirm our findings from 3D running analysis data, to better understand gait anomalies and how to correct them. It also alerts us to old injuries that were never properly rehabilitated, that contribute to gait anomalies. With this knowledge in hand, we are able to provide you with a comprehensive treatment plan that addresses all factors that influence your gait mechanics.


Your 17-page gait analysis summary report includes recommendations for enhancing your running performance. Our team of running specialists is available to provide personalized running physical therapy, injury rehabilitation, and running gait retraining.
Our team can provide you with:

ForceFrame is a comprehensive system for accurately testing and training isometric strength in various muscle groups throughout the body. Most people – especially physically active people – develop muscle imbalances and compensation patterns over time that reduce movement efficiency.
ForceFrame lets us test individual muscle groups on both sides of the body for strength and symmetry. By testing individual muscle groups isometrically, we eliminate the potential for compensation of weak muscles that could be masked during compound exercise testing.
The results of each test appear as objective data on a screen in real time, helping us to identify and correct muscle imbalances, asymmetrical muscle strength, inefficient muscle firing patterns, and compensation patterns developed from past injuries. We then use that data to create personalized rehab programs, to boost performance and reduce injury risk.
According to Yale Health, upwards of 50% of runners sustain injuries each year. And one study projected that up to 85% of novice runners experience a running injury while training for an event in any given year.
Many runners ignore seemingly minor injuries, continuing to run with bandaged knees and ankles, treating residual pain with OTC solutions and basic first aid. But failing to address minor injuries can lead to major problems down the road.
Most running injuries occur in the lower extremities and involve bones and connective tissues in the foot, ankle, knee and hip. Most are due to repetitive overuse and inefficient gait mechanics.
Common running injuries include:
Ignoring running pain and injuries can lead to gradual degeneration of tissues and create compensation patterns that set you up for more serious injuries down the road. While pain and dysfunction in runners is not uncommon, it is neither normal nor necessary. Early holistic treatment is essential to prevent life-long problems that cause disability as you age.
Our 3D motion analysis system gives us a broad range of quantitative data
about your running gait:
analyzes pressure and force related to foot mechanics.
measures joint angles during specific phases of the gait cycle, along with the timing of movement in bilateral joints.
measures ground reaction forces and weight distribution.
is a new technology that lets us visualize muscle and joint action in real time. This helps us confirm our findings from gait analysis data.
collects and interprets gait analysis data and produces a personalized report.

Gait analysis in three dimensions is a quantum leap forward in running analysis. In the past, gait analysis was mostly observational, and running gait could only be assessed in the frontal and sagittal planes. However, the majority of running injuries occur in the transverse plane — the third dimension that can only be assessed using advanced technologies.
The RunDNA system collects quantitative data that takes the guesswork out of gait analysis. Your personal running data is analyzed and presented to you in an easy-to-understand report that clearly pinpoints your running deficits. We then use that information to help you fine-tune your running performance.
Results from your 3D RunDNA gait analysis can help you:
Your RunDNA results can help you better understand how strength and flexibility affect your running gait. Your report helps us personalize a gait retraining program that puts you on the road to peak performance.
Once we have a clear picture of your running gait mechanics, we create a personalized gait retraining program to help you perfect your running gait. We use your objective baseline data to target specific mechanical deficits and measure your progress. Our advanced technologies leverage VR and AI to provide intrinsic and extrinsic feedback, to help you zero in on your unique running mechanics.
By fine-tuning your running gait, you can expect to prolong your years of pain-free running, avoid common injuries, and reach new performance heights.

Repetitive overuse injuries are common among runners, and early treatment is key to preventing more serious problems. NYDNRehab features a variety of advanced regenerative technologies that reduce pain and inflammation and speed up the healing process. Early intervention can prevent new and minor overuse injuries from becoming more serious conditions that keep you from running long-term.
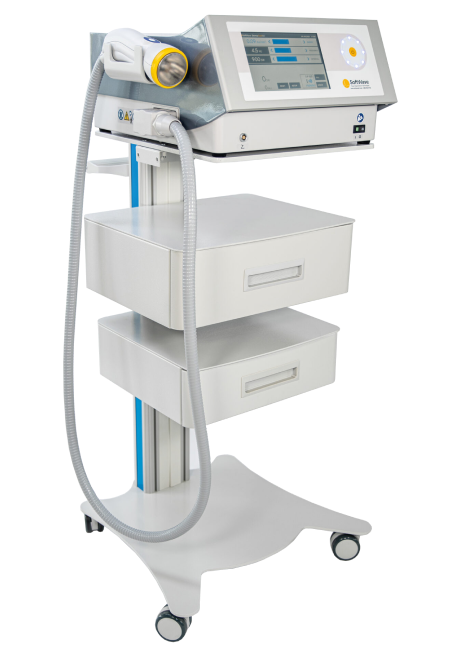
SoftWave is a groundbreaking regenerative mechanotransduction technology that accelerates tissue healing. Its patented electro-hydraulic applicator delivers high-speed soundwaves that can penetrate up to six inches in depth. SoftWave’s defocused and linear focused shockwaves recruit maximum stem cells to the treatment site to promote healing. SoftWave’s wider and deeper penetration using defocused energy is a preferred treatment option for a broad spectrum of conditions, ranging from orthopedic injuries to pelvic health. SoftWave is the only unfocused shockwave technology currently available. According to recent research, SoftWave defocused waves combined with focused and radial shockwaves have maximum regenerative potential.
MyACT is a new type of focused shockwave technology that allows for deeper compression of the focused waves. Its higher frequency allows for precise neuro modulation under ultrasound guidance, with a special linear head for treating myofascial pain. MyACT transforms the mechanical energy of shockwaves into biochemical signals that precisely target damaged tissues. Most injuries involve more than one tissue type. When used together, our advanced shockwave technologies enable us to specifically target multiple tissue types with the most effective shockwave treatment.
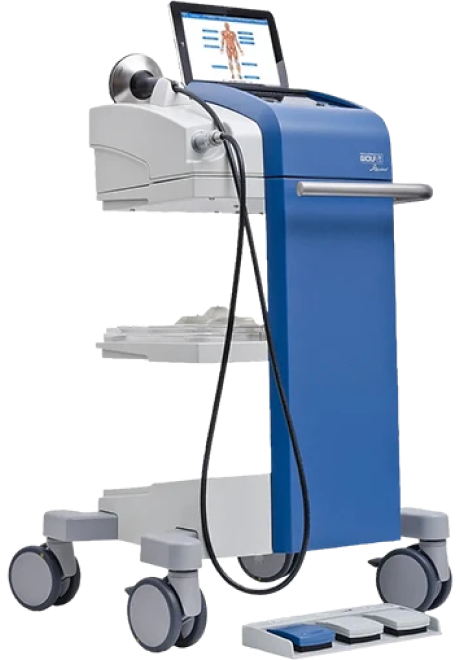

Focused ESWT is used as a regenerative treatment for damaged tendon, muscle and bone tissue. This technology produces high frequency sound waves to stimulate the body’s own reparative mechanisms. It is especially effective for chronic degenerative tendon disorders and myofascial pain syndrome.
EMTT transmits high energy magnetic pulses to targeted tissues that synchronize with the body’s own magnetic fields, triggering a regenerative response. EMTT waves can penetrate deep tissues to target difficult-to-reach tendons, muscles, bones and nerves.


EPAT, sometimes called defocused shock wave therapy, is not a true shockwave. It uses mechanical pressure waves to enhance blood circulation, improving oxygen and nutrient delivery to muscle and fascia tissues, but has minimal regenerative properties.The mechanical properties of EPAT make it especially effective for fascial manipulation in combination with focused shockwaves. We combine EPAT with different types of shockwaves for holistic treatment, without additional cost to the patient.
HEIT delivers high-intensity magnetic pulses to peripheral nerve tissues, to stimulate neuroplasticity. We leverage this FDA-approved methodology to treat pain and regenerate nerve fibers, for enhanced motor control.


INDIBA is a form of TECAR therapy that helps to restore the ionic charge of damaged cells, for faster injury healing and rehabilitation.
NESA generates a low-frequency electrical current of intermittent and cyclical stimuli that soothes hypersensitized nerves and restores optimal signaling between the autonomic nervous system and the brain. We leverage this FDA-approved methodology to treat pain and regenerate nerve fibers, to enhance motor control.

Injection therapies use orthobiologic solutions that stimulate cellular repair by either nourishing or irritating the targeted cells. Guidance by ultrasound ensures that the injected substances hit their mark, for maximum effectiveness.
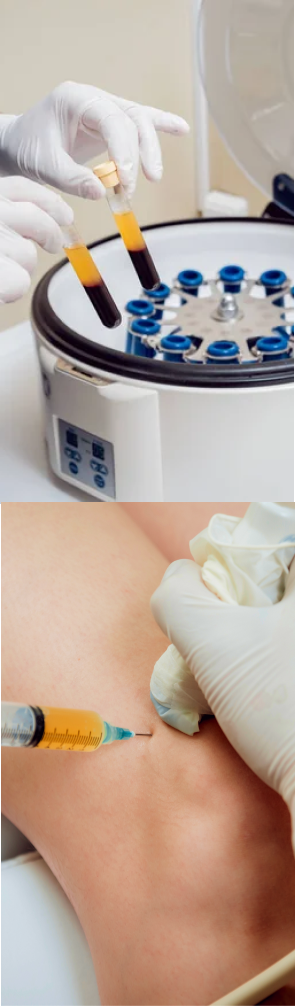
PRP therapy uses a sample of the patient’s own whole blood, which is spun in a centrifuge to extract a high concentration of platelets. When injected into damaged tissues, PRP initiates tissue repair by releasing biologically active factors such as growth factors, cytokines, lysosomes and adhesion proteins. The injected solution stimulates the synthesis of new connective tissues and blood vessels. PRP can help to jump-start tendon healing in chronic injuries and accelerate repair in acute injuries.
Alpha 2 macroglobulin (A2M) is a naturally occurring blood plasma protein that acts as a carrier for numerous proteins and growth factors. As a protease inhibitor, A2M reduces inflammation in arthritic joints and helps to deactivate a variety of proteinases that typically degrade cartilage.
Prolotherapy uses a biologically neutral solution to irritate stubborn tissues, triggering the body’s innate healing mechanisms to grow new normal tendon, ligament and muscle fibers.
Running injuries often involve fascial tissue that has become densified and/or formed adhesions, entrapping nerves and blood vessels, causing pain and restricting movement. Hydrodissection is a procedure where a saline solution is injected into densified fascia under ultrasound guidance. The solution works by separating fascial layers and freeing up entrapped nerves and blood vessels. We often use hydrodissection in conjunction with manual fascial manipulation.

SM neuromuscular electrical stimulation (NMES) dynamically interacts with the patient during therapeutic exercises, providing real-time sensory, auditory and visual biofeedback to the patient. This breakthrough technology helps patients to recalibrate muscle actions, to optimize joint function. SMNMES has helped numerous patients to avoid unnecessary shoulder, knee and ankle surgeries, even in complex scenarios.
During PENS treatment, filament-thin needles are inserted through the skin into muscle tissue adjacent to the targeted nerve. A low frequency electrical current is then delivered via the inserted needles to stimulate the dysfunctional nerve. PENS normalizes nerve activity, improves brain plasticity and optimizes muscle recruitment patterns. This therapy is so effective that patients typically need only 4-6 treatment sessions.
Advancements in technology are changing the game in rehabilitative medicine, enabling us to accelerate healing and restore performance at an unprecedented pace. The clinic at NYDNRehab features some of the most advanced therapeutic equipment currently available, and rarely found in private clinics.
Your running physical therapy may involve the use of high-tech equipment:

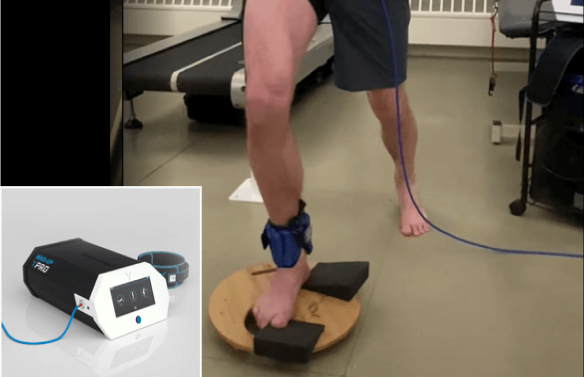


Before we get started on gait correction, we first need to prepare your muscles, joints and connective tissues, to ensure optimal results. We use dynamic high-resolution ultrasound to visualize your body’s structures in motion, to detect mobility issues that are invisible to the naked eye.


Despite advancements in shoe technology and massive amounts of available research on gait mechanics, injuries remain common among regular runners. According to Yale Medicine, 50 percent or more of runners get injured each year. Some injuries occur from trauma, but most are attributed to repetitive overuse.
Follow these guidelines to reduce your risk of running injuries:
