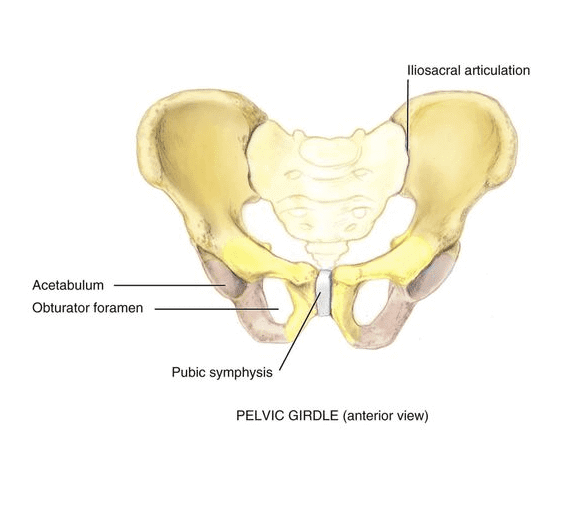
The Integrated Systems Model (ISM) is a model for treatment of pain and disability that applies to the whole person, and not just to a specific area of pain or injury. ISM is most often used in treating conditions that frequently occur in the pelvic region of women, including:
However, ISM is not limited to female pelvic disorders, but has applications for a broad range of disorders across all populations. As its name implies, the integrated systems approach recognizes that the body’s systems do not function independently of one another, but rather work together in an integrated fashion.
Originally presented as the Integrated Model of Function in 1998 and later as the more evolved System-Based Classification for Failed Load Transfer in 2007, ISM’s designers sought to provide a way for clinicians to get a multidimensional picture of each patient, so that an individualized multi-modal treatment plan could be designed.
In 2014 the latest iteration of the model appeared as ISM. The authors modified the model because they wanted to move away from the notion of classification, as it tends to place patients in homogenous subgroups, rather than treating them as unique individuals. ISM offers a framework to facilitate health care providers in understanding and interpreting the unique needs of individual patients.
ISM takes a whole-body approach that considers the articular, myofascial, neural and visceral systems (joints, muscles, nerves and organs). But ISM moves beyond a structural analysis, providing a flexible whole-body model that is able to adapt to the changing goals and values of the individual patient, while taking into consideration the patient’s emotions and needs.
The end goal of ISM to tell the patient’s story, so that appropriate and effective treatment can be initiated.
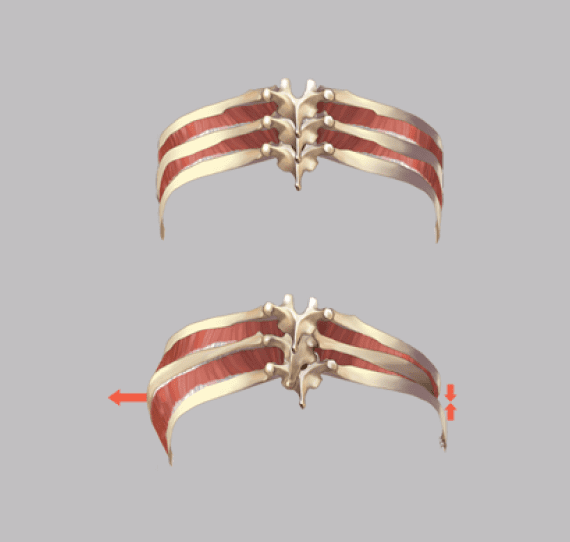
Your life experiences, family, friends and lifestyle have a far-reaching influence on your health over time. Physical pain that does not stem from trauma or overuse may have its roots in longstanding habits, behaviors or beliefs that have been overlooked or ignored. Oftentimes, painful and debilitating conditions arise when we move through life without examining or correcting things that collectively result in changes in strategies for posture, movement, organ support and continence. Poor postural habits, past injuries, emotional states and thoughts or belief systems can profoundly affect the way we move, sit and stand, which in turn affects how our body’s systems align and interact.
The way in which different individuals experience and react to pain or illness is unique, influenced by sensory, cognitive and emotional components that shape who they are. ISM clinicians factor in those three dimensions when creating a profile of the whole patient. Understanding the individual patient aids practitioners in making decisions and determining treatment.
For example, a practitioner may prescribe a detailed home exercise program for a patient with pelvic pain. Yet some patients will not be compliant with the treatment plan, while others will follow it to a tee. Knowing in advance that a patient is unlikely to be compliant with a home exercise program would no doubt influence the practitioner’s decision-making when devising a treatment protocol.
ISM is not a treatment method. It is an approach to evaluating a patient’s condition based on multiple factors, not just on the locus of pain.
ISM provides a framework for clinicians to organize information, to help them make the best decisions for treatment. Patients are assessed in various postures, based on the nature of their complaint. The objective is to identify factors that negatively affect whole body alignment, biomechanics and control that result in less-than-optimal load sharing and weight distribution throughout the entire body.
In order to identify the area where treatment should be focused, practitioners need to understand the interrelationships between the body’s systems and regions. An impairment in one region can have a profound impact on another, due to poor alignment, inefficient movement patterns, and poor control of and coordination between different body parts.
A clinician can use the ISM model to trouble-shoot key factors underlying a specific patient complaint.

Most human movement is not isolated, meaning that multiple systems are involved in everyday movements. For example, when you move from sitting to standing, you are transferring the load of your body weight from the chair to your feet, legs, hips, pelvis and trunk. In the process, the muscles of each of those areas are engaged in a coordinated series of contractions that eventually lead to a standing posture.
However, over time, some muscles can become overly lax and weakened, while others may become excessively tight, creating an imbalance in muscle tension. When you perform a particular movement, muscle imbalance can result in inefficient load transfer, causing some areas to bear more than their fair share of your body weight. This in turn can cause misalignments in the body’s structures that place pressure on neural bodies, limiting their free movement and causing pain.
During a patient assessment, an ISM clinician will look for failed patterns in load transfer to identify which site fails first, second, third and so on. They may attempt to manually correct the various sites to see how one failed site impacts other sites. For example, the clinician may ask you to perform a squat to detect deviations from optimal body mechanics. They will then note how those deviations interrelate, and determine the primary region that appears to be affecting the overall function of your entire body.
The ISM model is compatible with the holistic approach we take at NYDNRehab to treating pain and restoring optimal physical function. ISM is just one tool in our toolbox to help us accurately assess, diagnose and treat pain, injuries and movement dysfunction. We then design an individualized treatment plan aimed at correcting faulty movement patterns and restoring optimal function.
Some diagnostic and treatment methods used by the NYDNRehab team include:
Our team has access to the latest technological innovations for diagnosis and treatment, right in our Manhattan clinic. You do not have to live with chronic pain, or be resigned to a life of pharmaceutical interventions. Contact NYDNRehab today, and let us help you eliminate pain and restore function, so you can live your life to its fullest.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: