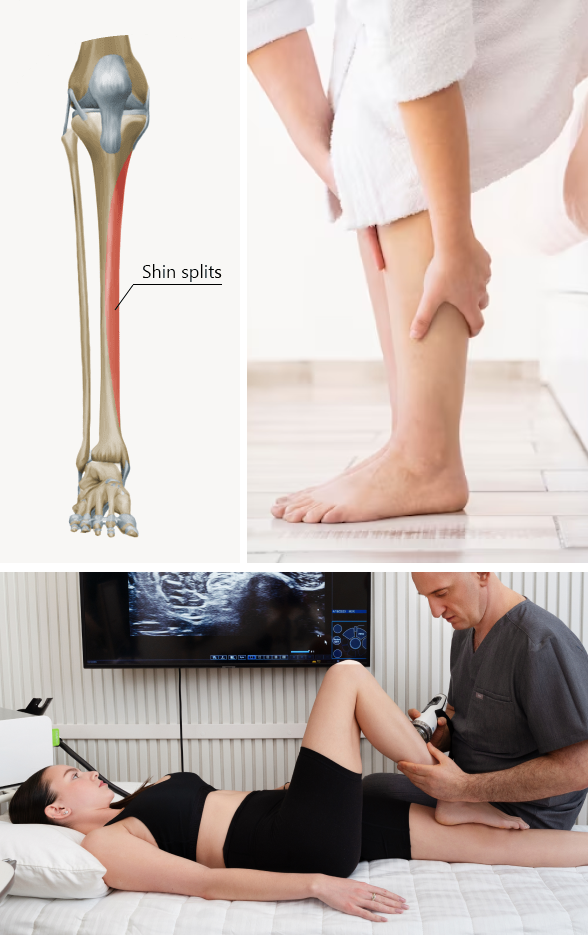
Shin splints are a fairly common sports injury that affects the front of the shin along the lower tibia. Shin splints involve inflammation of the muscles, tendons, and bone tissue that runs the length of your tibia. Pain typically occurs where the tibialis muscle attaches to bone, along the tibia’s inner border.
Shin splints are most common among military recruits, dancers and runners — especially novice runners. They also occur in athletes whose sport involves repetitive stress to the lower extremities. Shin splint pain can range from mild to debilitating. Early treatment and shin splint physical therapy can help to accelerate healing and prevent future injury.
or
Dr. Kalika has dedicated his life’s work to revolutionizing the way musculoskeletal pain and injuries are diagnosed and treated. Early training with some of the world’s most renowned human movement scientists set him on the path to finding new and innovative solutions for pain syndromes, movement disorders and injury rehabilitation. Along the way, Dr. Kalika has published multiple scientific papers, making a significant contribution to the body of research on rehabilitative medicine.
Dr. Kalika is certified in musculoskeletal ultrasonography, extracorporeal shockwave therapy (ESWT), dry needling, Dynamic Neuromuscular Stabilization (DNS) and many other therapeutic approaches. He works with elite athletes, runners and ballet dancers, along with everyday patients who want to move better, without pain or disability.
NYDNRehab is a top-rated NYC sports medicine clinic located in Midtown Manhattan. The clinic features some of the most advanced technologies for physical therapy, sports performance training and injury rehab in NYC.
At NYDNRehab, our personalized one-on-one approach sets us apart from mainstream physical therapy clinics. We never use cookie-cutter treatment methods or generic timelines to treat sports injuries. Our treatment protocols are case-specific, based on your unique condition and diagnostic results.
Conventional physical therapy clinics often rely on symptoms alone to diagnose shin injuries. However, a symptoms-based approach can overlook critical factors, leading to misdiagnosis and inappropriate treatment that prolongs the patient’s pain and can even do further damage.
At NYDNRehab, we use high-resolution diagnostic ultrasonography to generate dynamic images of the lower leg in real time. Ultrasound lets us detect serious conditions like stress fractures and tumors that require specialized therapy and condition-specific treatment protocols.
Our high-tech performance lab equips us with tools for 3D gait analysis, to detect and quantify motor deficits that are often the root cause of shin splints. We use VR and AI technologies to retrain gait patterns, to restore neural pathways between the brain and muscles, and optimize muscle firing patterns.
Our data-driven approach ensures that our patients get measurable results in the least amount of time. Our personalized treatment approach aims to restore functional movement and optimize performance while reducing your risk of re-injury, so you can return to your favorite sport with confidence.

Tibial stress fractures
Bone bruising
Bone tumors (rare)
At NYDNRehab, we use the highest-resolution ultrasound equipment available to get real-time images of your lower leg. Dynamic ultrasound imaging lets us view the structures of your leg in motion, along the entire path of the tibia. Ultrasound enables us to detect stress fractures and tumors that cannot be detected by X Ray or MRI. Our state-of-the-art ultrasound equipment gives us capabilities for sonoelastography, to measure the density of damaged tissues and monitor the healing process.
Once pain and inflammation have been addressed, we move to our performance lab for 3D gait analysis and biomechanical assessment. We look at joint angles, weight distribution, muscle firing patterns, and other mechanical indicators, in all 3 planes of motion, and create a personalized retraining strategy based on your unique data.

Shin splints can be extremely painful and debilitating — follow these common-sense steps to avoid them:
If you start to feel shin pain, apply ice and take a break from your sport or activity for a few days. If pain persists, seek professional help. Early intervention can spare you from a worsened condition that keeps you on the bench.

Living in a concrete jungle like NYC can take a toll on your body, and the impact of running on concrete can be hard on your shins. At NYDNRehab, our modern technologies are designed to quickly reduce pain and inflammation, and to stimulate your body’s reparative mechanisms at the cellular level.
But don’t wait for shin splints to appear — contact NYDNRehab today to get a 3D gait analysis, and fix your running mechanics to avoid common running injuries like shin splints. Take advantage of our high-tech performance lab, to stay at the top of your game and reduce your risk of injury.
If you think you’ve developed shin splints, it’s a good idea to stop the activity that caused them for 2-3 days. Apply ice to relieve pain and swelling, and elevate your lower leg to reduce inflammation. Remember, 90% of shin splint healing is load management (rest). If pain persists after a few days, seek professional shin splint treatment.
Training through pain is never a good idea – it can lead to acute compartment syndrome, a serious condition that can cause permanent deformity, disability, and infection. As much as possible, try to space out your training sessions, and apply ice immediately afterward. Elevate your legs and get as much rest as possible. You may also benefit from regenerative therapy leading up to and after your race.
While ankle range-of-motion exercises and gentle stretching may help promote healing, excessive walking is probably not a good idea. Rest, ice, compression and elevation are your friends in the early stages of soft tissue injuries like shin splints.
The tibialis anterior muscle often contains significant myofascial trigger points, which often go under-diagnosed and under-treated. Trigger points can sometimes be detected by palpation – you can feel tiny hard knots just below the skin’s surface. But deep tissue trigger points can only be detected with ultrasound imaging. Ultrasound guided dry needling is a fast and effective treatment for shin splint trigger points.
Independent peer-reviewed research relevant to this treatment approach.