October 8, 2024
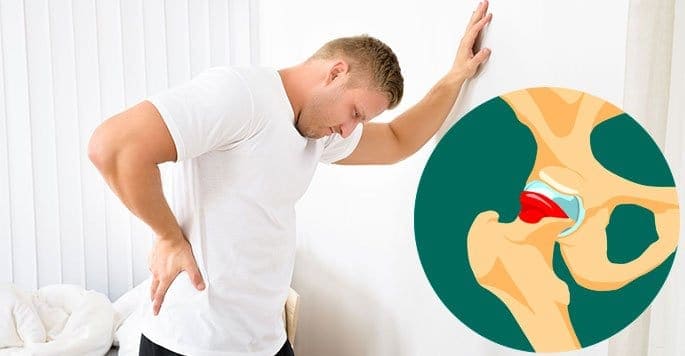
Regardless of your age, hip pain can be debilitating. The hip joint is one of the most complex joints in the body. It is also critical to get around successfully.
There are many different things that can cause hip pain. The potential causes include strains, osteoarthritis, referred pain from other joints, inflamed bursa and femoroacetabular impingement (FAI). Any of these can require professional treatment. Conservative treatment would start with noninvasive approaches, such as physical therapy.
That last condition is the one we will focus on here and it is a big word, so let’s start by breaking it down and explaining what the means. The hip is a ball-and-socket joint. Femur is the medical word for the thigh bone. The together. Outside of the medical profession, most people would just say “hip.” The femur plus the acetabulum make up the hip joint. Impingement just means that something is interfering with the normal range of motion for the joint in question. It is not moving the way it normally would. It is being limited in some manner.
We have already talked about the bones involved — the femur and the acetabulum. However, a functioning joint in a living person involves more than just the two bones that meet in that area. There are also tendons, ligaments, cartilage, and muscles involved. All of those different kinds of tissues are necessary to make the joint work at all. They each have a different function in making it work, in making it move the way it does.
The tendons and ligaments basically serve as anchors for the muscles and other structures. You can think of them as similar to speak.
Cartilage provides essential cushioning so that the bones do not rub to function at all, but not so much that the hip becomes easily dislocated.
The muscles provide the motion. Because of the unusually complex range of motion of this joint, there are many muscles that get involved in making it work. Flexor and extensor muscles allow it towards each other.
There are also hip rotato ball and socket joints. You see something similar in the shoulder. Most joints in the body cannot do this. Most of the joints of the human body only bend and unbend. The hip is fairly unique in having a complex range of motion.
There are two important different categories of femoroacetabular impingement. The first kind is a pincer defect. This is a situation where there are bony growths on the acetabulum. This is seen in women more often than in men.
The second category is called a cam defect. This is a kind of slang and is short for camshaft. In this case, the excess bony growth is on the head of the femur. It is frequently seen in relatively young men. Unsurprisingly, this is frequently a sports-related issue.
One medical study of the causes of FAI involved 44 patients. Half of them were known to impairment of the function of the hip joint, as well as pain and discomfort, sometimes at relatively young ages.
Other studies have suggested that FAI is present in approximately 15 percent of people with no sympto arthritis.
Some of the issues seen in patients suffering from FAI include groin pain, knee pain, ankle pain and general leg pain. The problem in the hip can throw things out of alignment such that other muscles, joints, tendons and ligaments are stressed. Everything in the body is interconnected. If the hip has a serious problem, all joints, muscles and other tissues involved in ambulation will be impacted toms of a hip disorder is not hip pain but pain in one of the related joints.
Additionally, FAI limits motion of the hip. It can limit moderately or substantially. Depending upon the daily activities of the patient in question, this may or may not be obvious. Athletes may be far more aware of the limited range of motion than nonathletes, but that doesn’t mean a nonathlete is not impaired or limited by it.
Many people with FAI are between 20 and 40 years of age. In most cases, their pain and decreased range of motion can be traced back to provide adequate relief and healing of the issue.
Some of the things which a physical therapist will work on include strengthening of specific muscles that have been medically determined to ride horses. In many cases, after physical therapy has been concluded, such activities can be pursued without limitations and the patient can resume a full and active life.
Other options include low dose ultrasound, arthroscopy and arthroplasty. In cases where full recovery is not possible, recommendations can be made for how to do?
If someone has sympto determine how out of alignment the joints are and which muscles groups and tendons may be involved.
They may ask you sit in odd positions in a chair or stand in odd positions while they observe. They may measure the length of both legs. The legs should be the same length. A significant difference in leg length can suggest the tendons and ligaments of one leg have been shortened and the body is out of alignment. This can often be corrected with appropriate therapies. A difference in length can be an important clue to the causes of your hip pain and other related pain, such as referred pain involving one or both of the knees.
If a physical exam alone is not satisfacto interfere with hip motion and cause loss of internal rotation, as well as hip pain.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: