Rapid Relief and Speedy Recovery with Shockwave Therapy for Plantar Fasciitis
Pain in any part of your body can really slow you down, but nothing makes it harder to live your best life than pain on the bottoms of your feet. Conventional treatment for plantar fasciitis often entails stretching, steroids and expensive orthotics that only work with one pair of shoes, and do little to relieve your pain.
Today, modern technology and a better understanding of the nature of plantar fasciitis are revolutionizing the way plantar fascia pain is approached and treated. Learn how extracorporeal shockwave therapy for plantar fasciitis can reduce pain and bring about healing in just a handful of painless sessions.
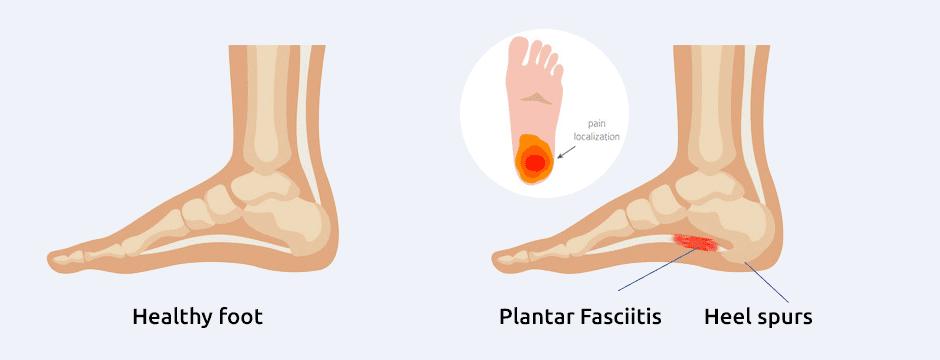
What is Plantar Fasciitis?
Plantar fasciitis is a painful condition affecting the tough elastic band of connective tissue running along the bottom of your foot, from your heels to your toes. It occurs when repetitive overuse, fatigue and structural imbalances cause microtears and stress to the plantar fascia, causing it to become stiff and painful.
Symptoms of plantar fasciitis include:
- Stabbing heel pain that worsens after rest
- Pain and swelling around the heel
- Pain that extends from the heel to the foot arch
- Pain that intensifies when standing or walking
As part of your foot arch complex, the plantar fascia stores elastic energy when stretched, much like a rubber band, releasing it as the band shortens to help propel you forward during the gait cycle. Plantar fasciitis causes the plantar fascia to become stiff and inelastic, inhibiting its ability to contribute energy to the gait cycle.
Common factors that contribute to plantar fasciitis include:
- Faulty mechanics in walking or running gait
- Repetitive actions like running and jumping
- Standing for extended periods on concrete or other unforgiving surfaces
- Unsupportive or poorly fitting footwear
- Postural issues that unevenly distribute body weight
- Imbalanced alignment of the lower kinetic chain
- Being overweight or obese
Plantar fasciitis occurs when one or more of these factors causes the plantar fascia to overstretch, creating micro tears in its fibers, similar to the way a rubber band becomes frayed after repetitive stretching.
Conventional Treatment of Plantar Fasciitis
Like most connective tissues, the plantar fascia is mostly made up of longitudinally arranged collagen fibers. As such, it has limited vascularity, restricting the inflow of oxygen and nutrients, and making injured tissues slow to heal.
Conventional treatments seek to reposition the foot in relation to the ground and the lower kinetic chain. This is done with orthotics — custom-made corrective shoe inserts — along with taping, bracing, stretching exercises, and physical therapy. Rest and elevation are also recommended.
Treatment may also include NSAIDs and corticosteroid injections to relieve pain and reduce inflammation. However, conventional therapy often provides only short-term pain relief, without fully resolving the underlying causes of plantar fasciitis.
Extracorporeal Shockwave Therapy for Plantar Fasciitis
Today, exciting new regenerative technologies are emerging that rapidly relieve plantar fasciitis pain and dramatically accelerate healing.
Extracorporeal shock wave therapy (ESWT) is a completely non-invasive outpatient treatment approach that applies focused high frequency sound waves to the affected tissues, to trigger the body’s own reparative mechanisms.
ESWT is especially effective for chronic and degenerative conditions of tendons and other connective tissues, where low vascularity inhibits the healing process. Treatment is fast and painless, and many patients report significant pain relief after a single ESWT session.
A recent research review of 11 randomized controlled trials, involving a total of 658 participants, found ESWT to be effective for reducing pain and improving foot function in patients with chronic plantar fasciitis. The researchers concluded that ESWT can be an effective alternative to traditional plantar fasciitis treatment methods
Another study found that just five ESWT sessions performed every other day produced highly satisfactory results in trial participants, in terms of pain relief and improved foot function.
When compared to weeks or months wearing uncomfortable orthotics and taking harmful medications, ESWT comes out the winner for fast results with minimal discomfort.
ESWT for Plantar Fasciitis in NYC
When it comes to new technologies like ESWT, skilled and experienced practitioners are scarce, and many physical therapy clinics do not have the equipment or expertise to provide shockwave therapy for plantar fasciitis. In addition, ESWT is most effective when guided by ultrasound, to ensure that the shockwaves effectively penetrate damaged plantar fascia tissues.
The clinic at NYDNRehab in Midtown Manhattan features the latest regenerative technologies, including ESWT for plantar fasciitis. When coupled with the highest resolution musculoskeletal ultrasound equipment, our technologies are game changers for patients suffering from pain syndromes and movement disorders.
Don’t waste your time on ineffective and outdated treatment methods for plantar fasciitis that cost you time, money, and weeks of discomfort. Contact NYDNRehab today, and start healing right away, so you can get back to doing the things you love.
About the Author
Dr. Lev Kalika is clinical director of NYDNRehab, located in Manhattan. Lev Kalika is the author of multiple medical publications and research, and an international expert in the field of rehabilitative sonography, ultrasound guided dry needling and sports medicine Dr. Kalika works with athletes, runners, dancers and mainstream clients to relieve pain, rehabilitate injuries, enhance performance and minimize the risk of injuries. His clinic features some of the most technologically advanced equipment in the world, rarely found in a private clinic.
Resource:
Krishnan, Anup, Yogesh Sharma, and Sonu Singh. “Evaluation of therapeutic effects of extracorporeal shock wave therapy in resistant plantar fasciitis patients in a tertiary care setting.” Medical journal, Armed Forces India 68.3 (2012): 236.
Melese, Haimanot, et al. “Extracorporeal shock wave therapy on pain and foot functions in subjects with chronic plantar fasciitis: systematic review of randomized controlled trials.” Disability and Rehabilitation (2021): 1-8.