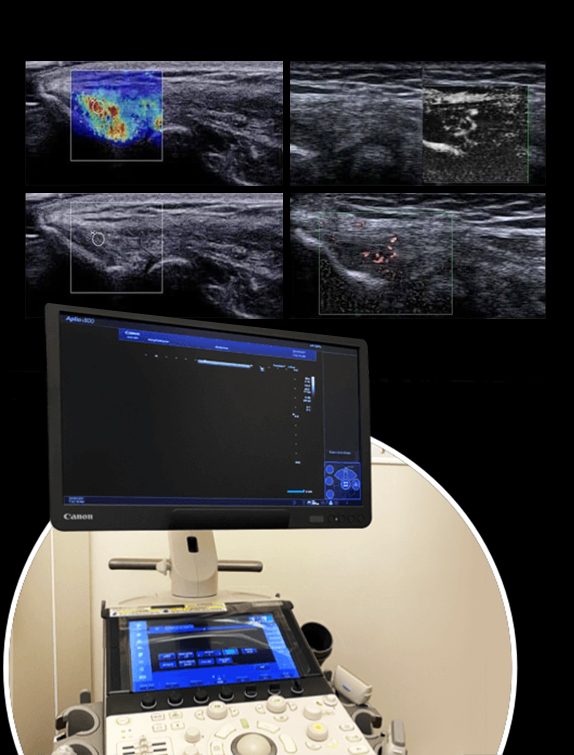
High Resolution Diagnostic Ultrasound Means Accurate Diagnosis and Successful Treatment
Because multiple structures converge at the elbow, it is impossible to know, based on symptoms alone, if your lateral elbow pain is caused by damage to the tendons that connect your forearm muscles to your elbow, or if other structural damage has taken place. In many cases, lateral elbow pain does not originate in the tendon, but arises from compression of the posterior interosseous nerve (PIN). Even when PIN compression is not the primary cause of pain, it can be a significant contributor. Pain can also be caused by instability of the lateral collateral elbow ligaments. In severe cases, multiple structures involving the elbow and forearm may be affected.
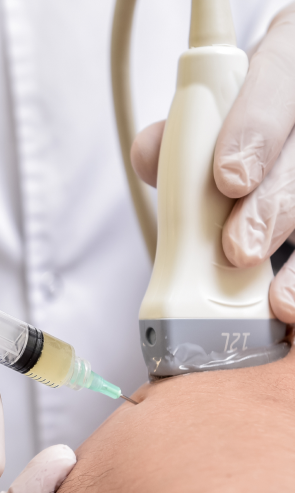
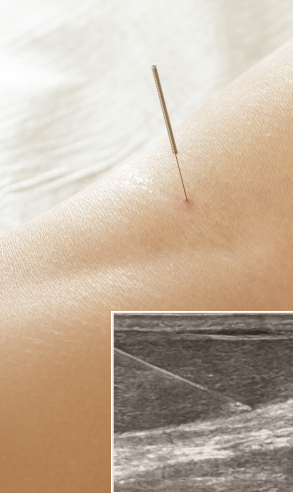
At NYDNRehab, we use the highest resolution diagnostic ultrasonography available, to closely examine the elbow and its surrounding structures. Ultrasound enables us to view the tissues in real time, with the elbow in motion, to rule out all possible causes of lateral epicondylar pain. With a precise and accurate diagnosis, we are able to provide the best condition-specific elbow pain treatment. Our use of regenerative technologies gives us nearly 100% success in resolving lateral elbow pain.