Patellar Tendonitis is a common athletic overuse injury, although it sometimes occurs in non-athletic populations. Your patellar tendon attaches your quadriceps muscles at the front of your thigh to your tibia (shin bone). During physical activity, the patellar tendon is subjected to great force loads as it straightens the knee during walking, running and jumping activities.
Patellar tendon dysfunction is sometimes called jumper’s knee due to its prevalence in sports that involve jumping. If left untreated, the tendon can begin to degenerate, leading to reduced mobility that can take you out of the game. New regenerative therapies and advanced technologies are able to halt patellar tendon degeneration and reverse it, to restore healthy tendon function.
or
Dr. Kalika has dedicated his career to revolutionizing the way musculoskeletal pain and dysfunction are diagnosed and treated. As a renowned tendon specialist, Dr. Kalika has developed his own unique approach to treating tendon injuries. The NYDNRehab clinic features some of the most advanced technologies available for diagnosing and treating pain syndromes and movement disorders.
Dr. Kalika is an expert in diagnostic ultrasonography and ultrasound-guided procedures. Our clinic features the most advanced high-resolution ultrasound equipment currently available, with capabilities for sonoelastography and superb microvascular imaging (SMI).
Elite athletes, runners and ballet dancers rely on Dr. Kalika’s expertise to heal and rehabilitate their injuries in the shortest time possible, so they can return quickly and safely to their sport or activity.
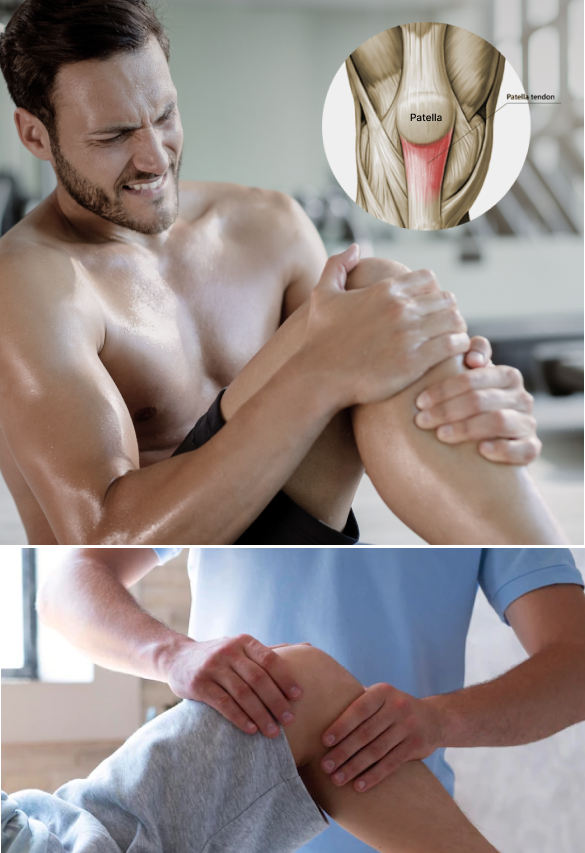
Athletes know that a knee injury can be a career-ending event if not properly rehabilitated. Run-of-the-mill physical therapy clinics staffed by inexperienced clinicians often prescribe one-size-fits-all treatment protocols that fall short of restoring peak functional performance.
At NYDNRehab, we take a personalized approach to patient care. We understand that every patient has a unique anatomy, and every injury has its own peculiarities. Our one-on-one approach ensures that you get a patellar tendonitis recovery plan designed just for you, so you heal and return to play in the shortest time possible.
We use regenerative technologies that accelerate patellar tendonitis healing time at the cellular level, for the fastest possible recovery. But we don’t stop there — we do biomechanical analysis and feedback retraining to restore neural pathways between your brain and body, to eliminate compensation patterns adopted after your injury.
Our cutting edge technologies let us quantify motor parameters and track your progress, eliminating guesswork and ensuring that you recover completely from your injury before returning to sport. Our goal is to return you to the playing field, faster, stronger and more confident than you were before your injury.
Symptoms
Patellar tendon pain
Lower kneecap tenderness
Swelling around your knee joint
Knee pain when jumping, running, or walking
Pain when bending and straightening your knee
Causes
Landing from a jump with an extended knee
Pivoting on a loaded knee
High velocity cutting and directional changes
Deficits in running gait mechanics
Inadequate recovery time between training sessions

Because patellar tendonitis shares symptoms with other knee conditions like torn meniscus or ACL ruptures, it is imperative to get an accurate patellar tendonitis diagnosis before starting treatment. A wrong diagnosis can lead to ineffective treatment that wastes your time and money, and the wrong treatment modalities can make your condition worse.
At NYDNRehab, we use the highest resolution diagnostic ultrasound to visualize the structures of the knee and surrounding tissues. Patellar tendonitis ultrasound is superior to Xray or MRI because it lets us visualize your knee in real time, with the patient in motion and providing feedback. Ultrasound lets us trace the path of long structures like bones, nerves and muscles, to look for damage that can prolong your patellar tendonitis healing time.
Our in-house high resolution ultrasound imaging lets us quickly confirm your diagnosis of patellar tendonitis without having to wait for lab results, so we can begin to rehabilitate your tendon right away.
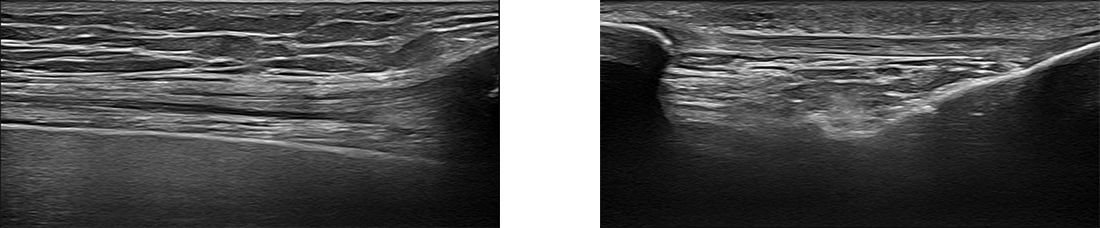
Please explore more advanced diagnostic option unavailable anywhere else:

Patellar tendonitis treatment protocols vary, depending on the condition of the affected tissues and the degree of degeneration. Early treatment focuses on reducing inflammation and stimulating the healing process. As healing progresses, you may receive some or all of the following therapies:
At NYDNRehab, we take an active approach to treating patellar tendinosis. Some of our treatment methods include:
Physical therapy for knee tendonitis
Dry needling of the patellar tendon
3D running gait analysis and retraining
Neuromuscular feedback training
Progressive eccentric loading
Blood flow restriction training
Ultrasound guided needling procedures
Regenerative therapies
Because tendons are made of tough collagenous fibers, they have limited vascularity, which can make them slow to heal. Regenerative therapies tap into your body’s innate healing mechanisms, creating an optimal environment for healing at the cellular level. Regenerative technologies are designed to jump-start the healing process and accelerate recovery, so you get the very best results in the shortest amount of time.
Focused ESWT is used as a regenerative treatment for damaged tendon, muscle and bone tissue. This technology produces high frequency sound waves to stimulate the body’s own reparative mechanisms. It is especially effective for chronic degenerative tendon disorders and myofascial pain syndrome.
EMTT is a fairly new technology that transmits high energy magnetic pulses to targeted tissues. The magnetic waves synchronize with the body’s own magnetic fields, causing a disturbance that triggers a regenerative response. EMTT waves can penetrate deep tissues up to 18 cm beneath the skin’s surface, to target difficult-to-reach tendons, muscles, bones and nerves.

Extracorporeal Pulse Activation Technology (EPAT)
EPAT, also known as defocused shock wave therapy, uses acoustic pressure waves to enhance blood circulation to targeted tissues. This speeds up the delivery of oxygen and nutrients to damaged tissues and stimulates cellular metabolism, to accelerate the healing process.
HEIT uses electromagnetic fields to penetrate cells, tissues, organs and bones, to reactivate the electrochemical function of cells and cell membranes. HEIT generates a magnetic field 600 times stronger than the field of a normal magnet, to stimulate healing of nerves, muscles and blood vessels.
Our INDIBA Tecar therapy machine converts electrical current into a stable radio frequency current of 448 kHz, designed to increase and stabilize the exchange of ions in damaged cells, evoking a regenerative response that accelerates healing. INDIBA can be used to successfully treat joint and muscle disorders, low-back pain, sports injuries, surgical incisions and various pain syndromes. Another therapeutic effect of INDIBA is extreme and prolonged cellular hyperthermia. Due to this effect, INDIBA therapy combined with manual therapy and soft tissue tissue manipulation enables instantaneous release to occur, significantly shortening the number and duration of physical therapy sessions. What is normally accomplished in two months of physical therapy can be accomplished in 3-4 sessions with INDIBA.

Injection therapies use natural/neutral solutions that stimulate cellular repair by either nourishing or irritating the targeted cells. Guidance by ultrasound ensures that the injected substances hit their mark, for maximum effectiveness.
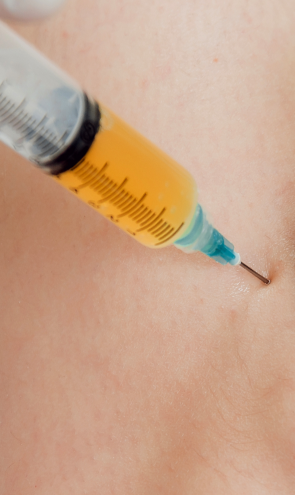
PRP therapy uses a sample of the patient’s own whole blood, which is spun in a centrifuge to extract a high concentration of platelets. When injected into damaged tissues, PRP initiates tissue repair by releasing biologically active factors such as growth factors, cytokines, lysosomes and adhesion proteins. The injected solution stimulates the synthesis of new connective tissues and blood vessels. PRP can help to jump-start healing in chronic injuries and accelerate repair in acute injuries.
Prolotherapy uses a biologically neutral solution, often containing dextrose, saline or lidocaine. The solution irritates the affected connective tissue, stimulating the body’s own natural healing mechanisms to encourage growth of new normal ligament or tendon fibers.
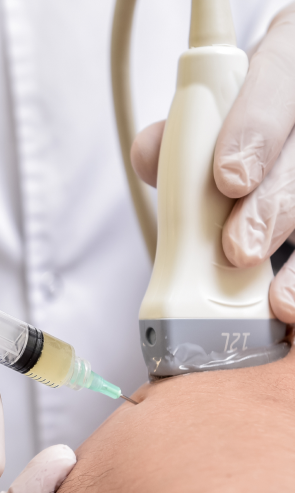
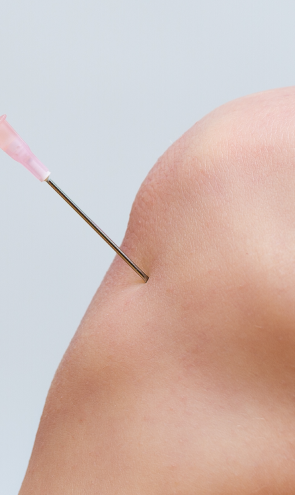
Myofascial trigger points often contribute to patellar tendon pain. Dry needling is an outpatient procedure where non-medicated needles are inserted into the trigger point to evoke a twitch response, releasing the trigger point and immediately relieving pain. Ultrasound guidance eliminates the need for multiple insertions, reducing pain and discomfort for the patient.
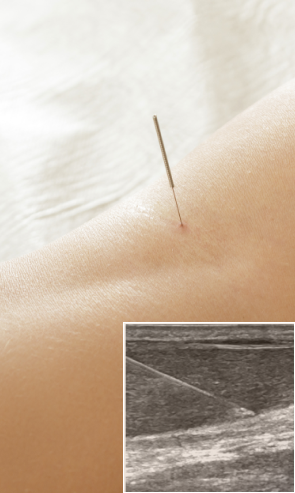
Patellar tendonitis often starts out with mild pain that intensifies over time. If left untreated, the tendon cells can begin to degenerate, causing loss of strength and function. Whether your tendon injury is fairly new, or it is an old injury that has begun to degenerate, the tendon specialists at NYDNRehab can help. Contact our team today, and see what a difference technology can make in rehabilitating your tendon injury.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including:Independent peer-reviewed research relevant to this treatment approach.
Research authored or co-authored by the clinic’s medical director. The following research publications inform the clinical approach used in this treatment program.