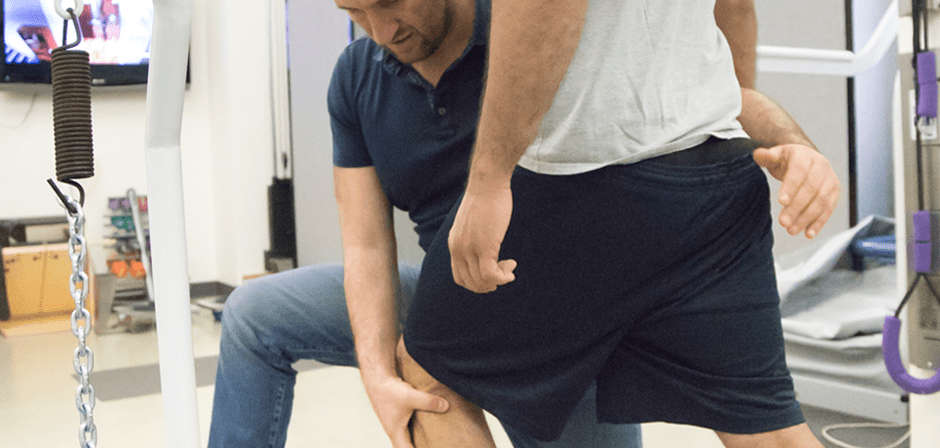
As the science of human movement progresses, we have increasingly more tools at our fingertips to assess, train and rehabilitate athletes, leading to higher performance levels and longer career spans. One growing area of interest is the role of the neuromuscular system in governing muscle recruitment patterns, which appear to be a contributing factor to knee instability and increased risk of ACL (anterior cruciate ligament) injury.
During any type of human movement, your musculoskeletal system responds to neural stimuli that tell your muscles when, in which order, and how forcefully to contract. Optimal movement requires a specific sequence of muscle activation patterns that accomplish motor skills with the greatest efficiency, and the least amount of effort.
In elite athletes, a well-trained neuromuscular system makes sport-specific motor skills appear fluid and effortless. The idiom, “practice makes perfect” was improved upon by legendary coach Vince Lombardi when he noted that “perfect practice makes perfect.” When applied to athletic training, we understand that repetitive skills training that develops optimal muscle recruitment patterns can lead to near-perfect execution during competition.
During sports like soccer, football and basketball that require rapid changes in direction, cutting, jumping and rapid deceleration, the knee absorbs enormous force loads. Optimal muscle recruitment helps to stabilize the knee in motion, protecting it from injury. Faulty muscle activation patterns can undermine knee stability, increasing the risk of ACL injury.
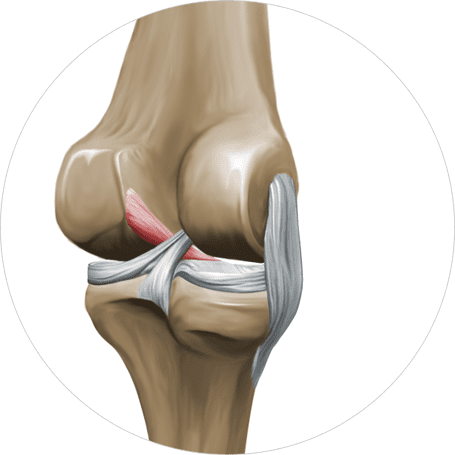
While skills training is essential to athletic performance, there are certain things that can interfere with optimal muscle activation.
Factors contributing to altered muscle activation may include:
Recently, researchers have found correlations between nociceptive response and altered muscle activation patterns in ACL injured athletes. The nociceptive reflex is response to a painful stimulus that causes withdrawal, similar to the way touching a hot surface causes you to reflexively withdraw your fingers. In the knee joint, the nociceptive reflex is characterized by an inhibition of the quadriceps and an excitation of the hamstrings.
During sports activities, the nociceptive reflex can alter leg muscle activation in ways that increases the risk of ACL injury.
A variety of tests may be conducted using gait, single and bilateral vertical drop jumps, squats, and other common motor skills.
Detecting sub-optimal muscle activation patterns in young or novice athletes can help therapists and coaches develop training programs that correct faulty muscle recruitment patterns and reduce the risk of injury.
Helping athletes reach their performance potential requires experience, knowledge and access to sophisticated technology that helps quantify the nuances of human movement.
The sports medicine team at NYDNRehab uses the latest technology for diagnosis, testing and rehab, including:

If you want to perform at your peak without fear of pain or injury, contact NYDNR today, and see what a difference technology can make in training and rehabilitation.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: