
Shin splints are a common lower leg injury affecting the front of the shin along the lower tibia. Shin splints are common among soldiers, runners and other athletes whose lower extremities are subjected to repetitive stress. Shin splints are also common among novice runners, and the condition can be so painful that new runners may be discouraged from continuing in the sport. Early treatment is key to healing shin splints, and to preventing the condition from becoming worse.
Although the term “shin splints” is used almost universally to describe sports-related shin pain, it is clearly not a very scientific name for a medical condition. In fact, “shin splints” is an umbrella term covering more than one type of shin injury.
The most common subcategories of shin splints include:
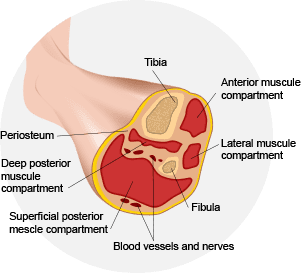
Compartment syndrome: Chronic compartment syndrome in the shin can develop from swelling or bleeding within a muscle compartment, made up of muscle fibers, capillaries and nerves surrounded by fascia. Because the fascia does not stretch, pressure builds within the compartment, reducing blood flow to the muscle and nerves.
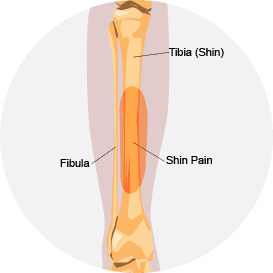
Medial tibial stress syndrome: Caused by inflammation where the anterior tibialis muscle attaches to the tibia, medial tibial stress syndrome accounts for 10 to 15 percent of running injuries, and 60 percent of lower leg pain syndromes.
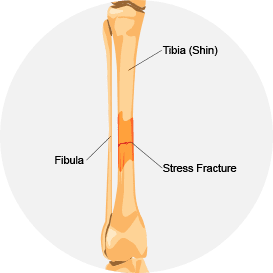
Tibial stress fracture: Fractures of the tibia can occur from repetitive stress, causing pain and inflammation. Stress fractures are often difficult to detect with Xray or MRI.
Shin splints are fundamentally a repetitive overuse injury, brought on by overtraining and inadequate recovery between training sessions. However, other factors may come into play that increase the risk of shin splints.
Reduced training and RICE (rest, ice, compression and elevation) can help alleviate shin splint pain.
Medical history and clinical exam are often the primary tools for diagnosing shin splints. Due to high inflammation, traditional imaging with Xray and MRI may not reveal the nature and extent of injury.
At NYDNR, we use real time diagnostic ultrasound to view the structures of your shins. Ultrasound imaging provides a clearer picture of stress fractures and other structural damage within the muscle compartment.
Reduced training and RICE first aid treatment can help alleviate shin splint pain. NSAIDs may also help reduce inflammation and pain. However, reducing pain will not correct the underlying causes of shin splints.
Orthotics are sometimes prescribed for people suffering shin pain, but their effectiveness is questionable. Well-fitting athletic shoes that provide support and shock absorption can help. Be sure to replace worn shoes frequently. A rule of thumb is to replace your running shoes every 300 to 500 miles.
At NYDNR, we use the latest technologies, including 3D motion capture video and force plate technology to analyze your gait and movement mechanics. We are then able to identify mechanical errors and correct them with C.A.R.E.N, our computer assisted rehabilitation environment.
Other treatment methods may include:
Shin splints can signal mechanical errors that may lead to more serious injuries down the road. Visit NYDNR today, and get to the root of your shin pain, so you can get back to the activities you love.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: