
Achilles tendinosis is a chronic degenerative condition that leads to scarring, hardening, and thickening of a tendon, causing pain and diminishing function. Tendinosis occurs when scar tissue forms in an injured tendon, characterized by abnormal collagen stands and irregular structural changes in cells, blood vessels and nerves as the body attempts to heal the damaged tissue.
If left untreated, a tendon injury, whether from trauma or overuse, can get progressively worse over time. But new Achilles tendinosis treatment technologies offer hope for patients suffering from Achilles tendinosis.
Tendons are tough soft tissues that attach your muscles to bones, creating a biomechanical lever system that allows you to move. As the muscle shortens, the tendon pulls on its associated bone, causing rotational joint action that produces movement.
Tendons are continuous with muscle, and share many of the same elastic and contractile properties, but as they approach the bone, they become increasingly collagenous. Tendon tissue is made up of 70-80% collagen.
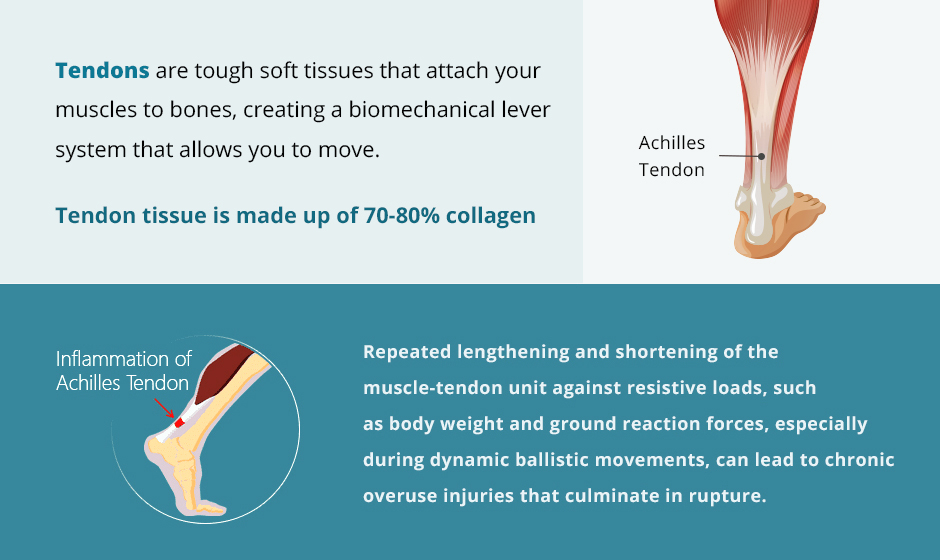
During the eccentric (lengthening) phase of muscle contraction, the Achilles tendon is stretched like a rubber band, storing elastic energy that is released during the concentric (shortening) phase, contributing significantly to force production.
Repeated lengthening and shortening of the muscle-tendon unit against resistive loads, such as body weight and ground reaction forces, especially during dynamic ballistic movements, can lead to chronic overuse injuries that culminate in rupture.
Tendon injuries are often slow to heal due to the low vascularity of tendon tissue that limits the amount of nutrients and oxygen that can reach the affected cells. A ruptured tendon can take several weeks to heal, or it may not heal at all, and instead degenerate into tendinosis that severely impedes performance and increases the risk of additional injuries.
Tendinosis arises from chronic overuse as a result of occupation, sports or exercise. Failure to allow for ample recovery time between training sessions or competitions is a significant contributing factor. Runners who train daily are at high risk. Chronic overuse often precedes a tendon rupture that is sometimes mistaken for an acute injury, but actually marks the advanced stages of repetitive overuse.
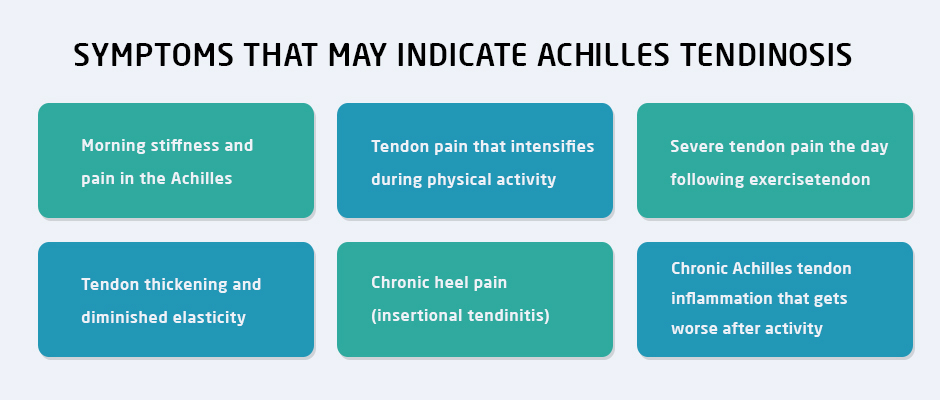
Symptoms that may indicate Achilles tendinosis include:
Morning stiffness and pain in the Achilles tendon
Tendon pain that intensifies during physical activity
Severe tendon pain the day following exercise
Tendon thickening and diminished elasticity
Chronic heel pain (insertional tendinitis)
Chronic Achilles tendon inflammation that gets worse after activity
Early treatment is key to effective healing. However, many people ignore Achilles tendinosis and continue doing the activities that cause it until the pain becomes unbearable. Others may discontinue their activities in hopes of healing but do not seek treatment, allowing the degenerative process to continue.
The diagnostic process begins with a thorough assessment of symptoms and patient history, but it doesn’t stop there. Recent advances in technology have given us tools to look beneath the surface, to get a more precise and accurate overview of the injury.
High resolution diagnostic ultrasonography allows us to visualize the Achilles tendon in real time, with the surrounding structures in motion, giving us a reliable picture of the type and extent of damage.
Sonoelastography enables us to assess the tendon’s elastic properties and compare them with the patient’s non-injured tendon.
Superior microvascular imaging lets us detect microscopic vascular activity that indicates that healing is taking place, and gives us a tool to assess the effectiveness of treatment.
A ruptured or damaged Achilles tendon can be career-ending for many athletes, especially if the injury was not adequately rehabilitated. At NYDNRehab, we leverage the latest technologies to optimize and accelerate the tendon healing process.
Our high-tech equipment lets us accurately measure your progress, to ensure your tendon is fully healed before you return to your active lifestyle.

ESWT stimulates the growth and repair of tissues at the cellular level. to accelerate healing for the fastest possible return to sports.
EMTT is making headlines as the next big thing in sports medicine and injury rehab. When combined with ESWT, EMTT helps to reduce inflammation, eliminate pain, and speed up the neogenesis of new tendon cells.
Dry needling is a safe and effective therapy for eliminating myofascial trigger points, often located near the bone-tendon junction. Guidance with ultrasound enhances precision, eliminating the need for repeated insertions.
We use ultrasound guided injections to reduce pain and inflammation and promote the growth of new cells. Corticosteroids, platelet rich plasma, hyaluronic acid and other injection therapies may be included in your treatment protocol.
This new technology enhances the effectiveness of evidence-based tendon loading protocols without doing further damage to injured tissues.
This multifaceted system gives us a broad range of options for testing, loading and retraining injured tendons, with a virtual reality feature for skills feedback training.
We use musculoskeletal ultrasonography as a tool for retraining optimal muscle firing patterns that often become altered after a tendon injury.
This elastic resistance suspension system takes isometric training to a new level, to promote tissue healing and restore tendon function.
While new treatment options offer great promise for healing Achilles tendinosis and restoring tendon function, very few sports medicine clinics have advanced technologies at their disposal for successful treatment.
The sports injury rehabilitation clinic at NYDNRehab embraces the latest technologies and most advanced treatment protocols for Achilles tendinosis treatment.
We provide our patients with the very best care, so you can get back into the game in the shortest time possible. Contact NYDNRehab today, and start healing now so you can get back out there!
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: