The tibialis posterior is a small but important muscle embedded deep in the lower leg that plays a key role in foot and ankle stability. Its insertional tendon contributes significantly to foot and ankle mechanics, helping to maintain the integrity of the medial longitudinal arch, and assisting in plantar flexion and foot inversion.
Early and aggressive treatment of posterior tibial tendinopathy can prevent its progression to dysfunctional chronic foot and ankle deformities. Regenerative technologies and specialized physical therapy can help to restore tendon integrity and promote optimal foot and ankle function and stability
During the loading phase of the gait cycle, the foot arch momentarily flattens and pronates (rolls inward) to provide shock absorption as the posterior tibial muscle lengthens, setting the foot up for the propulsion phase. The posterior tibial tendon dictates the speed and magnitude of pronation, which directly affects the mechanics of the entire lower kinetic chain.
Repetitive over-pronation can lead to injuries ranging from micro trauma to rupture of the posterior tibial tendon. If left untreated, an injured tendon may begin to degenerate, resulting in collapse of the medial arch and creating debilitating foot and ankle dysfunction that affects gait and posture.
or
With over 25 years of experience treating tendinopathies, Dr. Kalika has formulated his own unique approach to diagnosis and treatment. As an expert in diagnostic ultrasonography, he has published multiple scientific publications that have helped to take diagnostic medicine to the next level. He has worked with some of the world’s leading radiologists in the field of musculoskeletal ultrasonography.
“My success in treating tendon injuries comes from a deep understanding of tendon pathologies, and from the ability to visualize each individual tendon. No two tendons are alike in their anatomy, biomechanics and function. Most tendons are superficial structures, and are much better visualized by high resolution ultrasonography versus MRI. A distinct advantage of diagnostic ultrasonography over MRI is its ability to visualize muscles and tendons in motion.” – Dr. Lev Kalika
Dr. Kalika has helped hundreds of patients to rehabilitate tendon injuries, restore functionality, and return to sports and physical activity. Dr. Kalika’s expertise in musculoskeletal ultrasonography, shockwave therapy, regenerative medicine and 3D gait analysis makes him one of the most sought-after specialists in NYC for posterior tibial tendinopathy diagnosis and treatment.
NYDNRehab features research-grade ultrasound equipment with the highest resolution available in New York City. Our equipment gives us capabilities for sonoelastography to test for tendon stiffness, and superior microvascular imaging (SMI) to assess inflammation and detect vascular neogenesis.
Sonelastography and SMI are the latest advancements in tendon imaging, and are not possible with other radiological modalities. NYDNRehab is among the first sports medicine clinics to feature dynamic ultrasonography using the USONO ProbeFix device
ProbeFix attaches directly to the athlete, allowing us to visualize damaged tissues during sport-specific actions. ProbeFix renders accurate real-time images of the body’s structures in motion, and it can even be synced with motion capture cameras to produce 3D images of muscles, fascia, bones and joints during physical activity. This game-changing technology gives us a huge advantage for diagnosing tendon injuries and restoring optimal sport-specific biomechanics.NYDNRehab is the only clinic in New York with a fully equipped motion and gait analysis laboratory. Our motion and gait analysis technology and proprietary software lets us measure and quantify muscle and tendon function in real time.
At NYDNRehab, we are dedicated to rehabilitating your injury, not just treating your symptoms. To accurately diagnose and treat your tendinopathy, we conduct a comprehensive evaluation consisting of:
For sport-specific injuries, we use the latest technologies to analyze movement mechanics and identify motor deficiencies. By eliminating movement and training errors, athletes and physically active patients are able to dramatically improve their performance while reducing their risk of injury.


Patients with tendon injuries are often referred for MRI, but ultrasound imaging surpasses MRI in terms of visualizing tendons and surrounding structures in real time..

High-resolution ultrasonography not only gives us a cutting-edge diagnostic tool – it is a game-changer when it comes to tendon treatment. Most injuries involve multiple tissue types, and each demands its own therapeutic approach. Ultrasound imaging lets us differentiate between various tissues and structures to ensure that our needling and regenerative procedures hit their mark.
Ultrasound also provides a dynamic feedback tool for motor retraining. Injuries often disrupt optimal muscle coordination patterns when patients adopt compensation strategies to off-load injured tissues. Once the tissues have healed, it is necessary to restore neuromuscular pathways that govern motor unit firing patterns. Ultrasound gives the patient visual feedback, to help restore optimal muscle activation patterns.
In addition, ultrasonography helps us track and confirm the effectiveness of our treatment protocols. Its capabilities for sonoelastography and superb microvascular imaging let us detect early signs of healing, and dynamic real-time imaging lets us measure the patient’s progress toward restoring optimal mobility.
Most people take everyday mobility for granted until an injury occurs or pain sets in. Sometimes pain and reduced mobility seem to arise out of nowhere, with no apparent cause of onset. Regardless of whether your pain is caused by trauma or by something less obvious, tensegrity plays a key role.
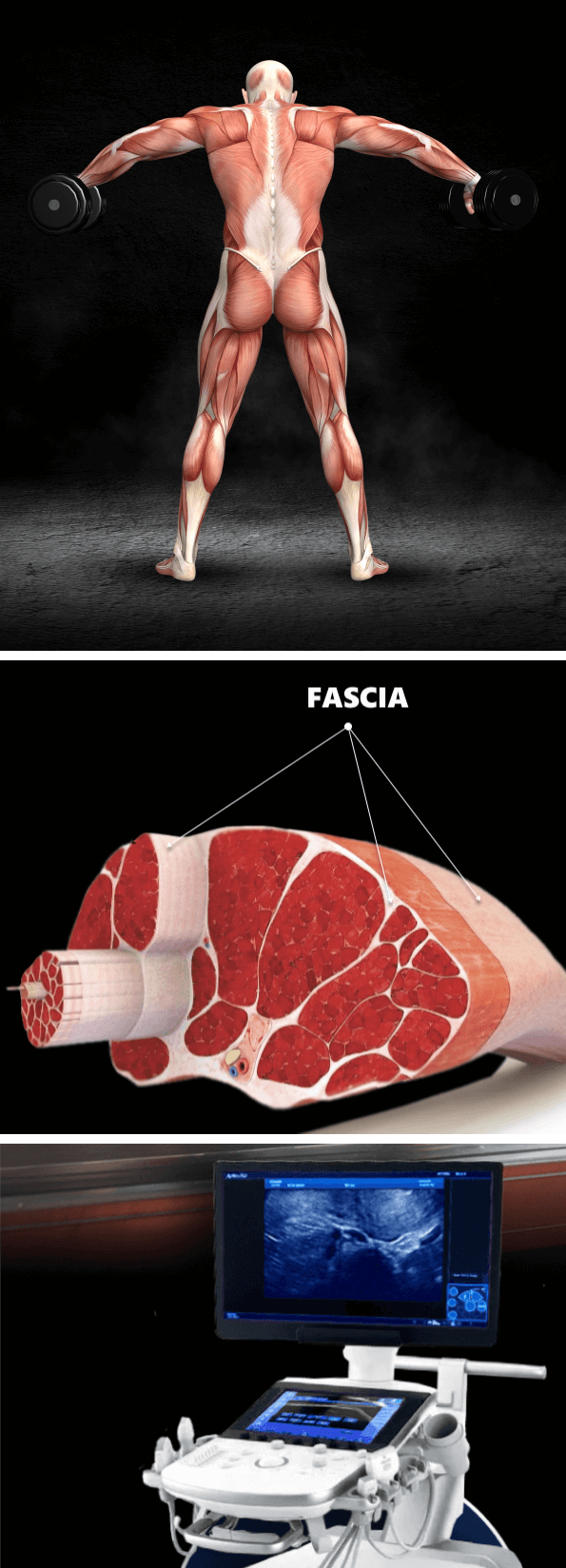
Tensegrity refers to tensile integrity – a state where a system of individual components is held together under continuous elastic tension. In the human body, tensegrity is created by the myofascial system, the network of muscles and fascia that work together to produce, control, and guide forces, and to hold the body’s various organs and structures in place during movement.
Tensegrity can be disrupted when myofascial tissues are injured or damaged in some way. When that happens, nerves and blood vessels can become entrapped, preventing them from gliding among other structures and producing pain. At the same time, the elastic tension that governs joint alignment and controls movement becomes compromised, creating motor deficits that undermine mobility and stability.
Factors that disrupt myofascial tensegrity include:
Many doctors do not understand the crucial role of the myofascial system in preventing pain syndromes, movement disorders, and disease. In fact, most medical doctors have no idea how to correct myofascial dysfunction or even recognize it as a factor. They simply treat pain symptoms with medications and eventually recommend surgery.
At NYDNRehab, we understand that the body’s systems work together as an integrated whole, and that treating pain is not enough to eliminate its source. We use dynamic high-resolution ultrasound to explore the myofascial system in real time. Ultrasound imaging lets us visualize muscles, fascia, nerves and other structures in motion, to identify places where tensegrity has been disrupted.
Once we identify the problem, we use the most advanced therapeutic approaches to restore myofascial integrity and promote tissue healing.
Physical therapy is an important component of tendon rehabilitation, but it does not provide a stand-alone solution. Prior to beginning physical therapy, we need to identify and treat complications that can undermine the effectiveness of physical therapy.
Issues that should be addressed prior to beginning physical therapy include:
Identifying and treating underlying issues prior to beginning physical therapy is key to getting fast and effective results. Failure to do so can completely undermine your treatment protocol, and in some cases your condition may even worsen.

The human body is made up of integrated parts and systems, designed to work in harmony. Today’s modern reductionist approach to medical treatment fails to acknowledge the integral relationship between structure and function, focusing on the locus of pain without considering its broader implications.
Most injuries involve multiple structures and tissue types, and pain is only a symptom that signals your brain to protect and heal the damaged tissues. It is not uncommon for an injury to stop hurting while damaged structures remain dysfunctional.
At NYDNRehab, our diagnostic process takes into account the interrelated nature of the body’s structures and systems, along with the unique anatomical characteristics of the individual patient. We use high resolution diagnostic ultrasound to visualize your injury dynamically, in real time, to determine whether structural (anatomical) changes are causing pain and dysfunction, or if dysfunction is causing structural changes.
Your ultrasound exam takes place on-site, on your first visit, where we examine multiple areas of the body in a single session – with no waiting for lab results!
The human body has its own innate healing mechanisms, but tendons sometimes need a nudge to accelerate the healing process. Regenerative technologies help to jump-start healing by stimulating tissue repair at the cellular level. Our outpatient regenerative therapies expedite recovery with minimal discomfort for the patient.
SoftWave is a groundbreaking regenerative mechanotransduction technology that accelerates tissue healing. Its patented electro-hydraulic applicator delivers high-speed soundwaves that can penetrate up to six inches in depth. SoftWave’s defocused and linear focused shockwaves recruit maximum stem cells to the treatment site to promote healing. SoftWave’s wider and deeper penetration using defocused energy is a preferred treatment option for a broad spectrum of conditions, ranging from orthopedic injuries to pelvic health. SoftWave is the only unfocused shockwave technology currently available. According to recent research, SoftWave defocused waves combined with focused and radial shockwaves have maximum regenerative potential.
MyACT is a new type of focused shockwave technology that allows for deeper compression of the focused waves. Its higher frequency allows for precise neuro modulation under ultrasound guidance, with a special linear head for treating myofascial pain. MyACT transforms the mechanical energy of shockwaves into biochemical signals that precisely target damaged tissues. Most injuries involve more than one tissue type. When used together, our advanced shockwave technologies enable us to specifically target multiple tissue types with the most effective shockwave treatment.

Focused ESWT is used as a regenerative treatment for damaged tendon, muscle and bone tissue. This technology produces high frequency sound waves to stimulate the body’s own reparative mechanisms. It is especially effective for chronic degenerative tendon disorders and myofascial pain syndrome.
EMTT transmits high energy magnetic pulses to targeted tissues that synchronize with the body’s own magnetic fields, triggering a regenerative response. EMTT waves can penetrate deep tissues to target difficult-to-reach tendons, muscles, bones and nerves.

Extracorporeal Magnetic Transduction Therapy (EMTT)

EPAT, sometimes called defocused shock wave therapy, is not a true shockwave. It uses mechanical pressure waves to enhance blood circulation, improving oxygen and nutrient delivery to muscle and fascia tissues, but has minimal regenerative properties.The mechanical properties of EPAT make it especially effective for fascial manipulation in combination with focused shockwaves. We combine EPAT with different types of shockwaves for holistic treatment, without additional cost to the patient.
HEIT delivers high-intensity magnetic pulses to peripheral nerve tissues, to stimulate neuroplasticity. We leverage this FDA-approved methodology to treat pain and regenerate nerve fibers, for enhanced motor control.


INDIBA is a form of TECAR therapy that helps to restore the ionic charge of damaged cells, for faster injury healing and rehabilitation.
NESA generates a low-frequency electrical current of intermittent and cyclical stimuli that soothes hypersensitized nerves and restores optimal signaling between the autonomic nervous system and the brain. We leverage this FDA-approved methodology to treat pain and regenerate nerve fibers, to enhance motor control.

Injection therapies use orthobiologic solutions that stimulate cellular repair by either nourishing or irritating the targeted cells. Guidance by ultrasound ensures that the injected substances hit their mark, for maximum effectiveness.
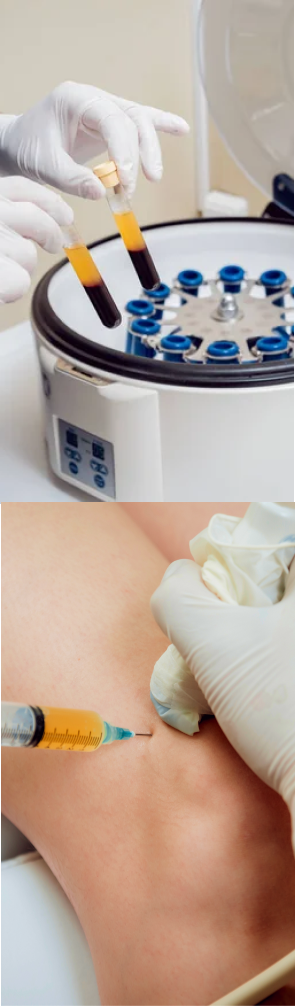
PRP therapy uses a sample of the patient’s own whole blood, which is spun in a centrifuge to extract a high concentration of platelets. When injected into damaged tissues, PRP initiates tissue repair by releasing biologically active factors such as growth factors, cytokines, lysosomes and adhesion proteins. The injected solution stimulates the synthesis of new connective tissues and blood vessels. PRP can help to jump-start tendon healing in chronic injuries and accelerate repair in acute injuries.
Alpha 2 macroglobulin (A2M) is a naturally occurring blood plasma protein that acts as a carrier for numerous proteins and growth factors. As a protease inhibitor, A2M reduces inflammation in arthritic joints and helps to deactivate a variety of proteinases that typically degrade cartilage.
Prolotherapy uses a biologically neutral solution to irritate stubborn tissues, triggering the body’s innate healing mechanisms to grow new normal tendon, ligament and muscle fibers.
Condition injuries often involve fascial tissue that has become densified and/or formed adhesions, entrapping nerves and blood vessels, causing pain and restricting movement. Hydrodissection is a procedure where a saline solution is injected into densified fascia under ultrasound guidance. The solution works by separating fascial layers and freeing up entrapped nerves and blood vessels. We often use hydrodissection in conjunction with manual fascial manipulation.

SM neuromuscular electrical stimulation (NMES) dynamically interacts with the patient during therapeutic exercises, providing real-time sensory, auditory and visual biofeedback to the patient. This breakthrough technology helps patients to recalibrate muscle actions, to optimize joint function. SMNMES has helped numerous patients to avoid unnecessary shoulder, knee and ankle surgeries, even in complex scenarios.
During PENS treatment, filament-thin needles are inserted through the skin into muscle tissue adjacent to the targeted nerve. A low frequency electrical current is then delivered via the inserted needles to stimulate the dysfunctional nerve. PENS normalizes nerve activity, improves brain plasticity and optimizes muscle recruitment patterns. This therapy is so effective that patients typically need only 4-6 treatment sessions.
While posterior tibial tendon dysfunction (PTTD) can develop in athletic populations, it is most prevalent in up to 10% of obese middle-aged women. Co-factors such as diabetes, hypertension, obesity, previous surgery, foot/ankle trauma and corticosteroid use are found in up to 60% of PTTD patients.
It is important to note that multiple other conditions share similar symptoms to PTTD, and misdiagnosis is not uncommon. Diagnostic ultrasonography gives us a superior tool for differentiating posterior tibial tendinopathy from imposters, ensuring you get the most effective treatment for your condition.
At NYDNRehab, we treat the whole patient, not just their symptoms. We never use one-size-fits-all rehab protocols or antiquated recovery timelines. We believe that every injury is unique, and treatment should be based on a holistic approach that factors in the patient’s unique profile.
Once we have successfully pre-treated damaged tissues, we can begin one-on-one physical therapy to restore strength and stability, optimize mobility, and re-establish optimal neuromuscular pathways and muscle coordination patterns.
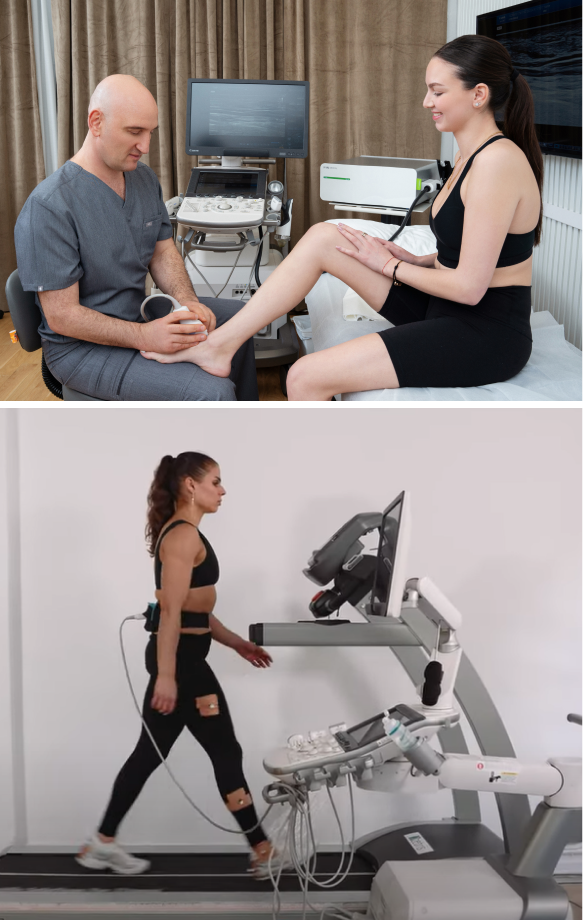
To restore functional movement during tibial tendinopathy rehab, we look at all the factors that play into lower kinetic chain mechanics. Our personalized approach ensures that every patient gets the exact physical therapy needed, based on their unique diagnostic profile.
Foot core training is a physical therapy approach for strengthening the intrinsic foot muscles that provide foot stability and arch support. Strong intrinsic foot muscles help to mitigate force loads placed on the posterior tibial tendon, prevent excessive foot pronation, and preserve the arch's capacity for storing and releasing elastic energy during the gait cycle.
Inefficient gait mechanics during walking and running can originate anywhere along the lower kinetic chain, affecting all other structures involved in the gait cycle. Our state-of-the-art gait analysis lab is fully equipped with advanced technologies for detecting and quantifying gait deficiencies that affect the posterior tibial tendon. Gait retraining uses intrinsic and extrinsic feedback to optimize gait mechanics.
Advancements in technology are changing the game in rehabilitative medicine, enabling us to accelerate healing and restore performance at an unprecedented pace. The clinic at NYDNRehab features some of the most advanced therapeutic equipment currently available, and rarely found in private clinics.
Your tendinopathy therapy may include the use of technologically advanced equipment:

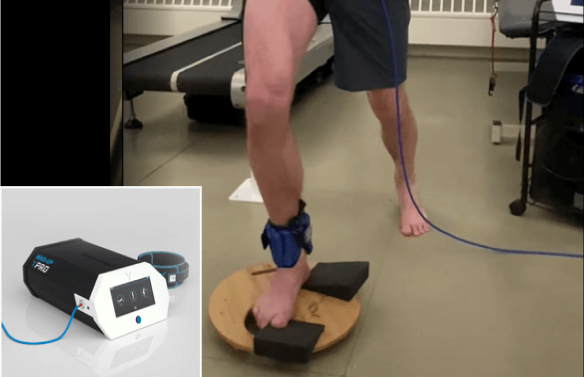


Certain uncontrollable factors can potentially increase your risk of a tendon injury:
Women have smaller tendons, with a lower capacity for hypertrophy due to lower protein turnover, lower levels of insulin-like growth factor (IGF-1), and less collagen synthesis in response to exercise. In addition, higher estrogen levels in females reduce tendon stiffness, potentially increasing injury risk.
The ability of tendons to store and release energy diminishes with age. Physical activities that load tendons to the point of fatigue have been shown to cause greater damage to the tendon matrix in older adults.
