Everyday activities are hard on your body, especially your feet and ankles. Sometimes pain arises for unknown reasons. It the pain is in your ankle, there is a good chance you have a condition called peroneal tendonitis. Each foot has two peroneal tendons that run parallel to each other behind the outer ankle bone. One attaches to the outer part of your midfoot, while the other runs beneath your foot and attaches near the inner arch.
Peroneal tendonipathy is common in sports that involve running or intense ankle loading, such as ice skating, basketball, football, and other sports that overload the feet and ankles. A sudden increase in mileage or increased athletic activity with excessive ankle motion can exceed the tissues’ load tolerance, causing the tendon to fail. The fibers then separate and loose their optimal integrity for managing resistance loads.
In medical terminology, words ending in “itis” mean that pain is caused by inflammation. However, in the case of the peroneal tendons, there is rarely inflammation, but rather a degeneration of the tendon tissue itself. It most often results from repetitive overuse, poor ankle stability or poor proprioception. Sometimes peroneal tendinopathy is misdiagnosed as a sprained ankle.
There are two clinical classifications of peroneal tendon injuries:
Acute injuries are caused by overuse or overload on the muscles, and include tears and ruptures. Injury occurs when a powerful contraction of the peroneal muscles is coupled with spontaneous dorsiflexion (toes up) of the foot. Acute injuries are common in people ages 20-35, often from athletics.
Chronic injuries are associated with weak and unstable ankles that cause issues with the peroneal tendons. Chronic injuries are often associated with aging, overuse, poor foot mechanics, poor balance, inefficient proprioception, and poor motor control.
Peroneal tendonitis is common in athletes whose activity involves running, such as ice-skating, basketball, football, and others. When there is sudden increase in mileage or other sporting activity with excessive ankle motion which exceeds the tissue tolerance, the tendon tissue fails. The fibers then separate and loose optimal integrity necessary for optimal load resistance and function.
Unlike an ankle sprain that causes pain and swelling, straining the peroneal tendons will cause pain during foot pronation and supination, without swelling. Pain will occur on the side or the back of the ankle, and may feel like it is wrapping around the ankle joint. Occasionally, pain may radiate up the leg.
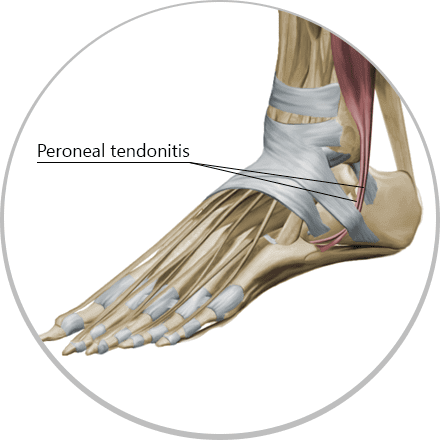
Pain in the foot is seen as swelling in the foot area and debilitation of the ankle in the area where the fibula bone has connection with peroneus tendons.
The main symptoms of peroneal tendinopathy include:

Several conditions can mimic peroneal tendinopathy, so imaging with MRI or ultrasound is necessary to confirm it.
At NYDNRehab, we use diagnostic musculoskeletal ultrasonography (MSUS) to view the structures of the foot and ankle. Unlike MRI where the patient stays perfectly still and results take several days, MSUS lets us view the injured tissues with the patient in motion, so we can observe the mechanics of the foot in real time and get immediate results.
Our clinic has the most powerful research-grade ultrasound equipment available in NYC. In addition to viewing the body’s structures, it enables us to perform sonoelastography and superior microvascular imaging to further assess the degree of damage and healing.
With diagnostic MSUS, the patient becomes an active participant in the diagnostic process, repositioning the injured area for a more comprehensive view, and providing verbal feedback about which movements cause pain or discomfort. Both patient and practitioner are able to view the results on the monitor, and discuss the degree of injury as well as potential treatment.
Explore more advanced diagnostic tools available only at NYDNRehab:
The main cause of the condition is excessive overuse from loading the ankle during physical activity. Inadequate warmup, improper training approaches and poor exercise technique may play a role. Faulty biomechanics is often a contributing factor.
Other causes include:
In the acute phase, ankle injuries should be treated with RICE (rest, ice compression and elevation). Over the counter NSAIDs like ibuprofen or naproxen may help reduce pain and swelling. Once swelling has abated, physical therapy can begin, to strengthen the peroneal tendons and surrounding musculature, with the goal of restoring full function.
Treatment may include:
NYDNRehab has some of the most advanced treatment technologies in the US for rehabilitating injuries and preventing them. If you are suffering from ankle pain, do not ignore it. Contact NYDNRehab today, and get back to moving freely, without pain.

At DNR we use gait or running analysis for precise diagnosis of biomechanical causes. We use diagnostic ultrasound to diagnose. We use state of the art rehab treatments and ESWT (extracorporeal shockwave therapy) for treatment of peroneal tendinitis.
Dr. Lev Kalika is a world-recognized expert in musculoskeletal medicine. with 20+ years of clinical experience in diagnostic musculoskeletal ultrasonography, rehabilitative sports medicine and conservative orthopedics. In addition to operating his clinical practice in Manhattan, he regularly publishes peer-reviewed research on ultrasound-guided therapies and procedures. He serves as a peer reviewer for Springer Nature.
Dr. Kalika is an esteemed member of multiple professional organizations, including: